Overview
Cone and cone-rod dystrophies are a group of genetically and phenotypically heterogeneous disorders. In cone dystrophy, the patients typically experience photophobia, reduced central vision, impaired colour vision, a variable degree of nystagmus and field loss. In cone-rod dystrophy, the patients also develop night blindness and peripheral field loss as the disease progresses. The onset of symptoms and the prognosis are variable.
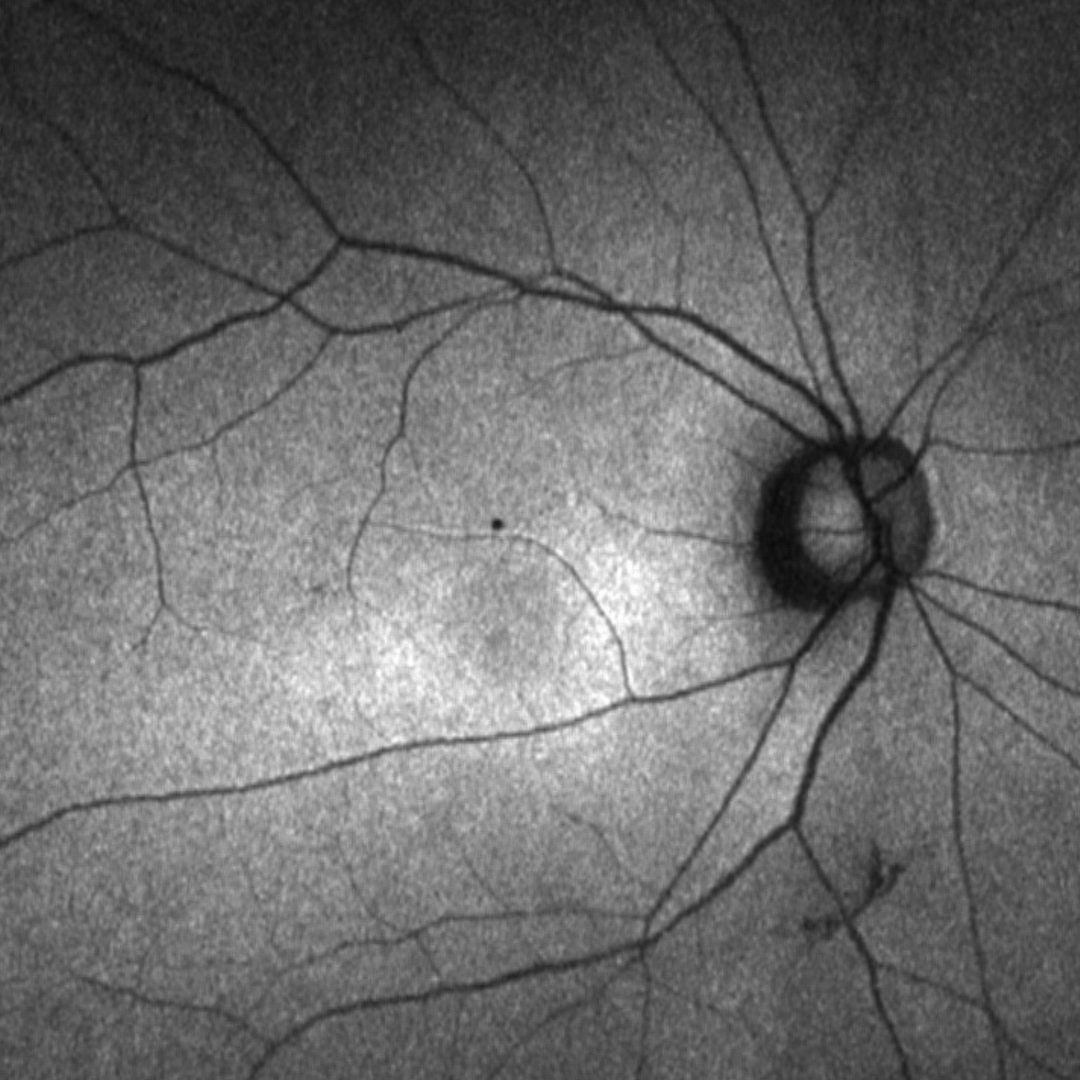
Funduscopy can reveal a classic bull’s eye maculopathy although in some cases, only mild RPE disturbance is noted. In cases of cone-rod dystrophies, peripheral RPE atrophy and bone spicule pigmentation may be observed.
Autofluorescence and OCT imaging results are variable.
Full-field ERG is the gold standard for diagnosis and shows reduced single-flash and flicker responses in photopic conditions and normal response in scotopic conditions in cone dystrophy and early cone-rod dystrophy. The scotopic responses are also compromised in the later stage of cone-rod dystrophy.
Case Examples
-
Case 1
A 67 year old Caucasian female with visual acuity of 6/24+ (20/80+) in the right eye and 6/24- (20/80-) in the left. Monocular colour vision testing showed 10 crossings in each eye, predominantly along a deutan axis.
Fundus photograph and red-free image (right eye)
More infoFundus photograph and red-free image (left eye)
More infoFundus autofluorescence (FAF) - right and left eye
More info10-2 SITA standard visual field
More infoSpectralis OCT volume and line scans (Right macula)
More infoSpectralis OCT volume and line scans (Left macula)
More infoElectrophysiology results
More info -
Case 2
A 15 year old male who reports having difficulties seeing the blackboard at school. Best corrected visual acuity is 6/12 (20/40) in each eye.
Colour vision testing
More infoFundus photographs (right and left eye)
More infoRed free images (right and left eye)
More infoFundus autofluorescence (FAF) images - right and left eye
More infoSpectralis OCT line scans (right macula)
More infoSpectralis OCT line scans (left macula)
More infoOCT macular thickness map
More info30-2 SITA standard visual field
More info -
Case 3
A 49 year old Asian male complaining of difficulty reading bus numbers and taking longer to adjust from dark to light. Also noted difficulty discerning some colours. Refraction showed high myopia with high astigmatism, confirmed by topography to be regular astigmatism. Pinhole acuities were 6/38+2 (OD) and 6/38 (OS). Low contrast VA (Mars contrast sensitivity 1.04 units RE, 1.20 units LE (normal 1.52-1.76)
Fundus photographs (right and left eye)
More infoFundus autofluoresence (FAF) imaging
More infoCirrus OCT line scans
More infoCirrus OCT macular line scan (OD)
More infoCirrus OCT macular line scan (OS)
More infoCirrus OCT Macular Thickness Map
More infoHumphrey 24-2 visual field results
More infoHumphrey 10-2 visual field results
More infoFull field electroretinogram (ERG)
More infoPattern ERG
More info
Differential Diagnosis (Bull's Eye Maculopathy)
Additional conditions not yet covered in this Atlas that should be considered in the differential diagnosis of bull's eye maculopathy are benign concentric macular dystrophy, Batten disease and Bardet-Biedl syndrome.
References
Gill JS, Georgiou M, Kalitzeos A, et al (2019) Progressive cone and cone-rod dystrophies: clinical features, molecular genetics and prospects for therapy. British Journal of Ophthalmology 103:711-720.