Overview
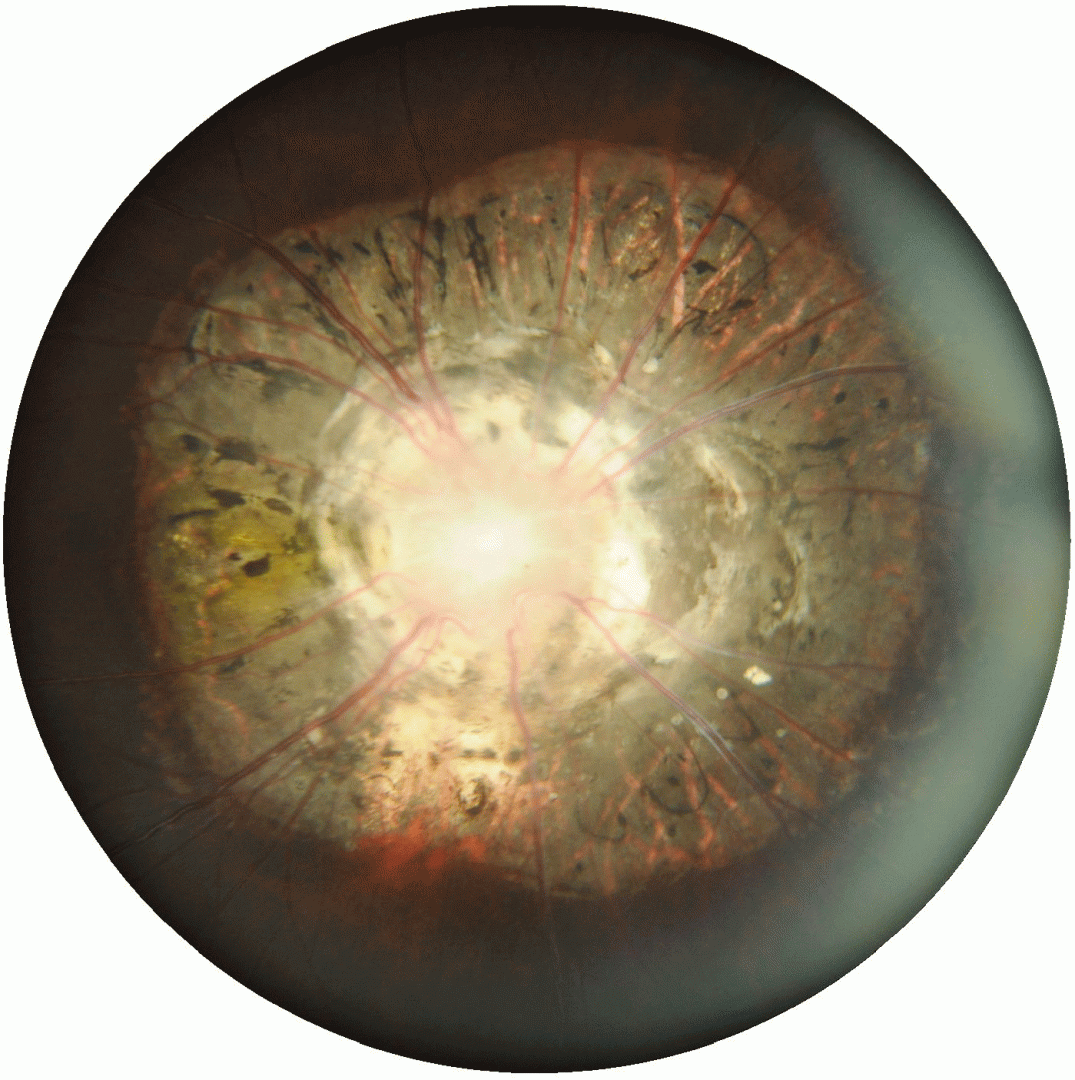
Morning glory syndrome is thought to arise from an abnormal closure of the embryonic fissure and is named after its resemblance to the flower of the same name.
This anomaly is characterised by a funnel-shaped excavation of the optic disc with straight, radial retinal vessels emerging from the disc. A white glial tuft is typically seen at the centre of the optic disc and the peripapillary region may show annular hyperpigmentation.
Approximately 50% of patients with morning glory syndrome may develop maculopathy or serous retinal detachment.
A variety of systemic and developmental conditions may be associated with morning glory syndrome. These can include midline craniofacial defects, neurocutaneous disorders, PHACE syndrome (which includes posterior fossa abnormalities, haemangioma and cardiovascular abnormalities amongst others).
Case Examples
-
Case 1
A 24 year old Asian female with best corrected visual acuity of 6/120 (20/400) in the right eye. The left eye was unremarkable so this case will focus on the right eye only.
-
Case 2
A 7 year old Caucasian male with best corrected visual acuity of 6/7.5 (20/25) an unremarkable medical history.
-
Case 3
A 35 year old Asian female with best corrected visual acuity in the right eye of 6/24 (20/80).
Differential diagnosis
References
Fei P, Zhang Q, Li J, et alClinical characteristics and treatment of 22 eyes of morning glory syndrome associated with persistent hyperplastic primary vitreousBritish Journal of Ophthalmology 2013;97:1262-1267.
Hu J. The clinical characteristics and imaging findings of morning glory syndrome. J Huazhong Univ Sci Technolog Med Sci. 2008 Aug;28(4):465-8.