- Overview
- Association with multiple sclerosis
- Prognosis
- Case Examples
- Differential diagnosis (papillitis)
- Differential diagnosis (previous optic neuritis)
Overview
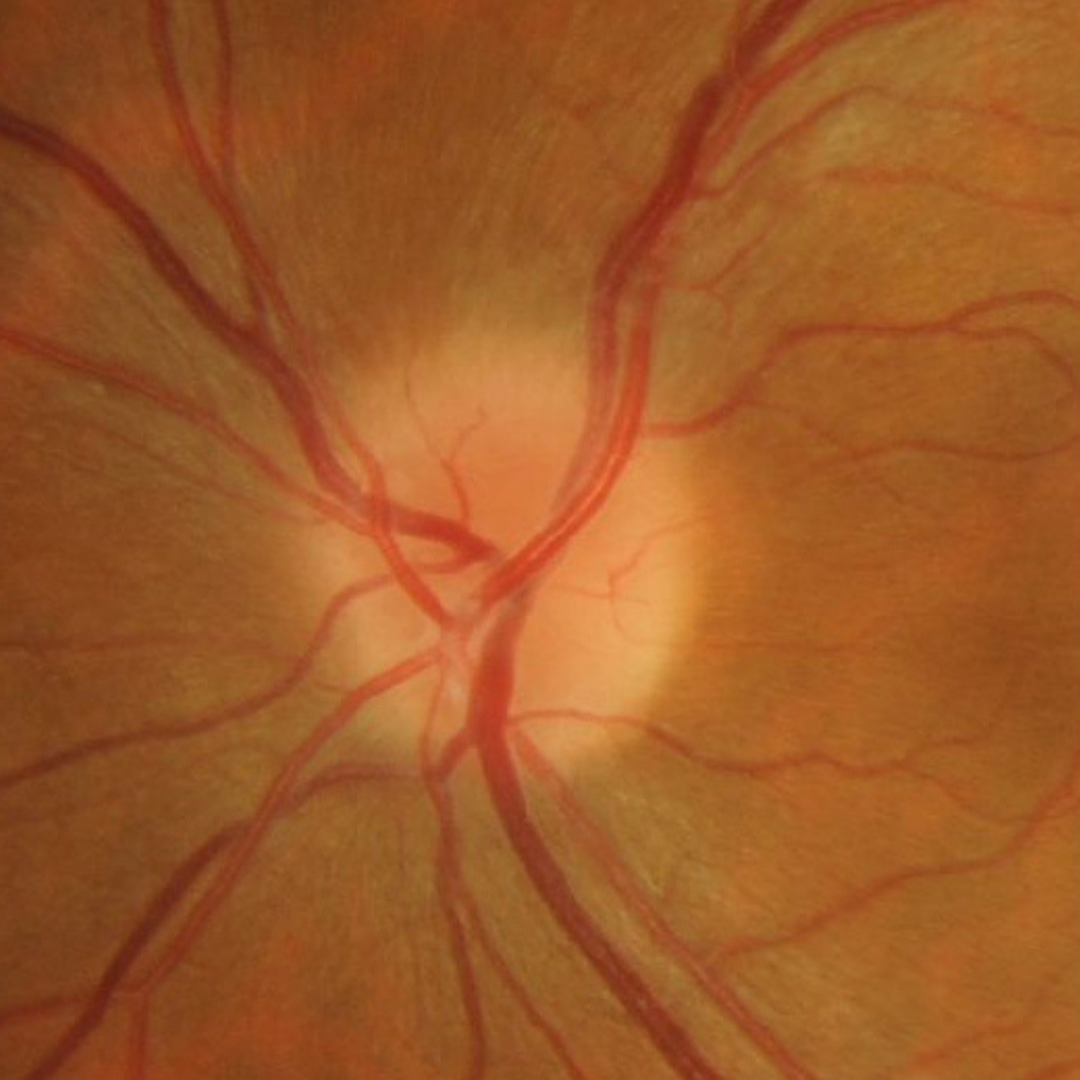
Optic neuritis is an inflammatory disease of the optic nerve, frequently associated with demyelination due to multiple sclerosis (approximately 50% of cases). However, it may also be associated with other autoimmune and inflammatory conditions including diabetes, neuromyelitis optica (NMO) spectrum disorder and chronic relapsing inflammatory optic neuropathy (CRION).
Optic neuritis affects women more than men and typically presents in those younger than 50 years of age. Affected individuals present with monocular vision loss occurring progressively over several hours to days and is typically accompanied by pain on eye movements. Red cap desaturation and relative afferent pupillary defect may be present in the affected eye. Visual field defects are variable, ranging from a general field depression and centrocecal scotoma through to altitudinal defects.
The signs and symptoms of optic neuritis may be exacerbated by an increase in body temperature (warm bath, exercise, fever etc), known as Uhtoff’s phenomenon. Patients recovering from optic neuritis may also note difficulty in depth perception when looking at moving objects (Pulfrich phenomenon).
Depending on the location of involvement, it may present with swelling and elevation of the anterior part of the optic nerve (papillitis) or with no visible funduscopic signs of inflammation (retrobulbar optic neuritis). Visible disc swelling occurs in approximately one half to one third of cases.
- In cases of papillitis, disc oedema and RNFL thickening can be seen initially.
- Retrobulbar optic neuritis is not associated with an acute elevation of the optic disc as inflammation is occurring more posteriorly along the nerve. The other signs and symptoms noted above however still occur including reduced vision, visual field defects, pain on eye movement and red desaturation.
Resolved optic neuritis of either type is associated with RNFL thinning, making it one differential to consider when making a glaucoma diagnosis.
Association with multiple sclerosis
The Optic Neuritis Treatment Trial (ONTT) showed a 5-year cumulative probability that a patient with optic neuritis would be diagnosed with multiple sclerosis was 30%. This risk however was highly dependent on the number of lesions present on brain MRI at first presentation. The study also found however that having no brain lesions present on MRI at first presentation did not preclude the development of multiple sclerosis (Neurology 1997).
Prognosis
Visual recovery was also monitored over time in the ONTT. Results showed that in 93% of cases, vision started to improve within 5 weeks of an acute presentation. 15 year follow up of patients in this study found that visual acuity and visual function was normal or near normal in most patients at that time but patients with multiple sclerosis were more likely to have deficits in normal visual function (Ophthalmology, 2008).
Case Examples
-
Case 1: Acute papillitis
A 45 year old Caucasian female reporting recent reduction in vision and photopsia in her left eye. Her best corrected visual acuity is 6/6(20/20) in the right eye and 6/7.6- (20/25-) in the left.
-
Case 2: Previous optic neuritis
A 53 year old Asian female with a history of optic neuritis at the age of 17. Her best corrected visual acuity is 6/7.5-2 (20/25-2) in the right eye and 6/9.5-1 (20/30-) in the left eye.
-
Case 3: Previous optic neuritis
A 46 year old female with history of optic neuritis in her right eye 23 years previously. Steroid medication was used 6 months. Her best corrected visual acuity is 6/9.5 (20/30) in the right eye and 6/6 (20/20) in the left. A red cap test showed even saturation between the two eyes and no RAPD was present.
Retinal photo and red free image (right eye)
More infoMagnified view of the right optic nerve
More infoCirrus RNFL analysis
More infoCirrus ganglion cell analysis
More infoCirrus PanoMap (right eye)
More infoOCT line scan (right eye)
More infoOCT angiography (right optic nerve)
More info24-2 SITA-Faster visual field (right)
More info