Overview
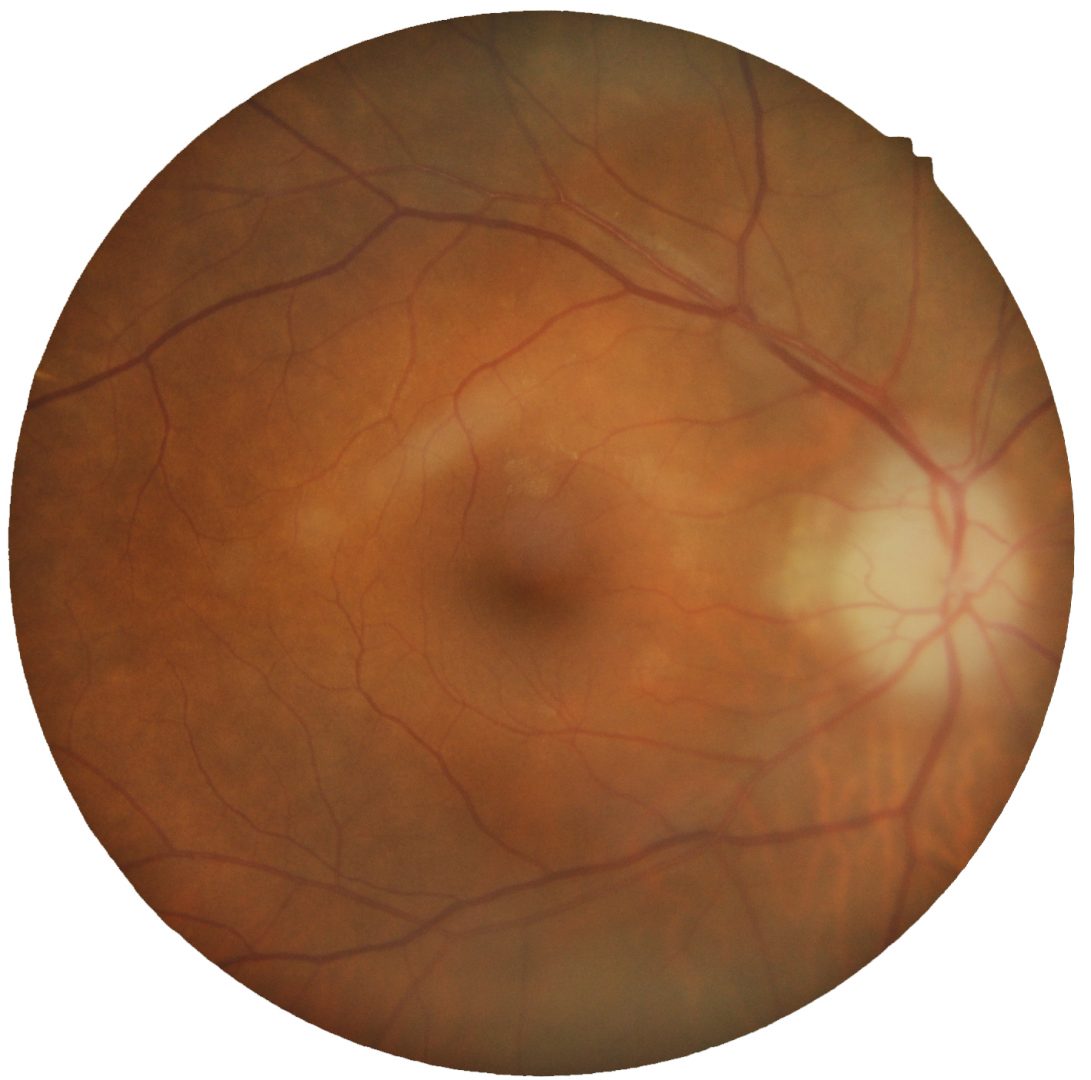
Arteritic anterior ischaemic optic neuropathy (AAION) arises from the obstruction of the posterior ciliary arteries due to inflammation. This obstruction is usually complete, so no blood flows to the optic nerve head. Subsequent ischaemia leads to a pallid swelling of the optic nerve head giving it a pale-white, elevated appearance. AAION is associated with very severe visual loss (hand movements or worse).
AAION is associated with giant cell arteritis (GCA), also known as temporal arteritis, which is a granulomatous vasculitis of the arterioles. Symptoms of GCA include a temporal headache, jaw claudication, scalp tenderness, fever and malaise.
AAION is a medical emergency as it is life-threatening. If left untreated, loss of vision in the second eye can occur. AAION may be difficult to distinguish from non-arteritic anterior ischaemic optic neuropathy (NAAION) however the presence of pallid disc swelling and severe vision loss are strong indicators of AAION.
Features include a chalky white oedematous disc with associated haemorrhages during the acute event. Bilateral optic nerve head pallor with associated cupping is the usual sequalae following the acute episode.
On OCT, marked thickening of the RNFL will be seen in the acute phase. The acute phase is usually followed by generalised atrophy of the RNFL and ganglion cell complex as the swelling dissipates. OCT-angiography may show superficial peripapillary capillary dilation in the acute stages followed by superficial peripapillary capillary attenuation in the chronic stages (Gaier et al. 2017)
Prognosis
Corticosteroid treatment aims to stop progression of the condition to the second eye and to prevent potential mortality, however it offers little chance of visual improvement
With corticosteroid treatment, only 10% of patients show an improvement in visual acuity of 2 lines or more, and only 4% of these also show an associated improvement in visual field (Acta Ophthalmologica, 2003)
Case Examples
-
Case 1
An 82 year old Asian female presents with sudden vision loss in the right eye. Patient was seen in emergency and was diagnosed with giant cell arteritis.
Visual field testing revealed an absolute, full field scotoma in the right eye. The visual field results for the left eye are provided below.
Fundus photographs (right and left eye)
More infoMagnified view of the right and left optic nerve head
More infoRed free images (right and left eye)
More infoCirrus RNFL analysis
More info30-2 SITA-standard visual field (left eye)
More infoFundus photographs at initial presentation and follow up (right eye)
More infoCirrus guided progression analysis (right eye)
More info