Overview
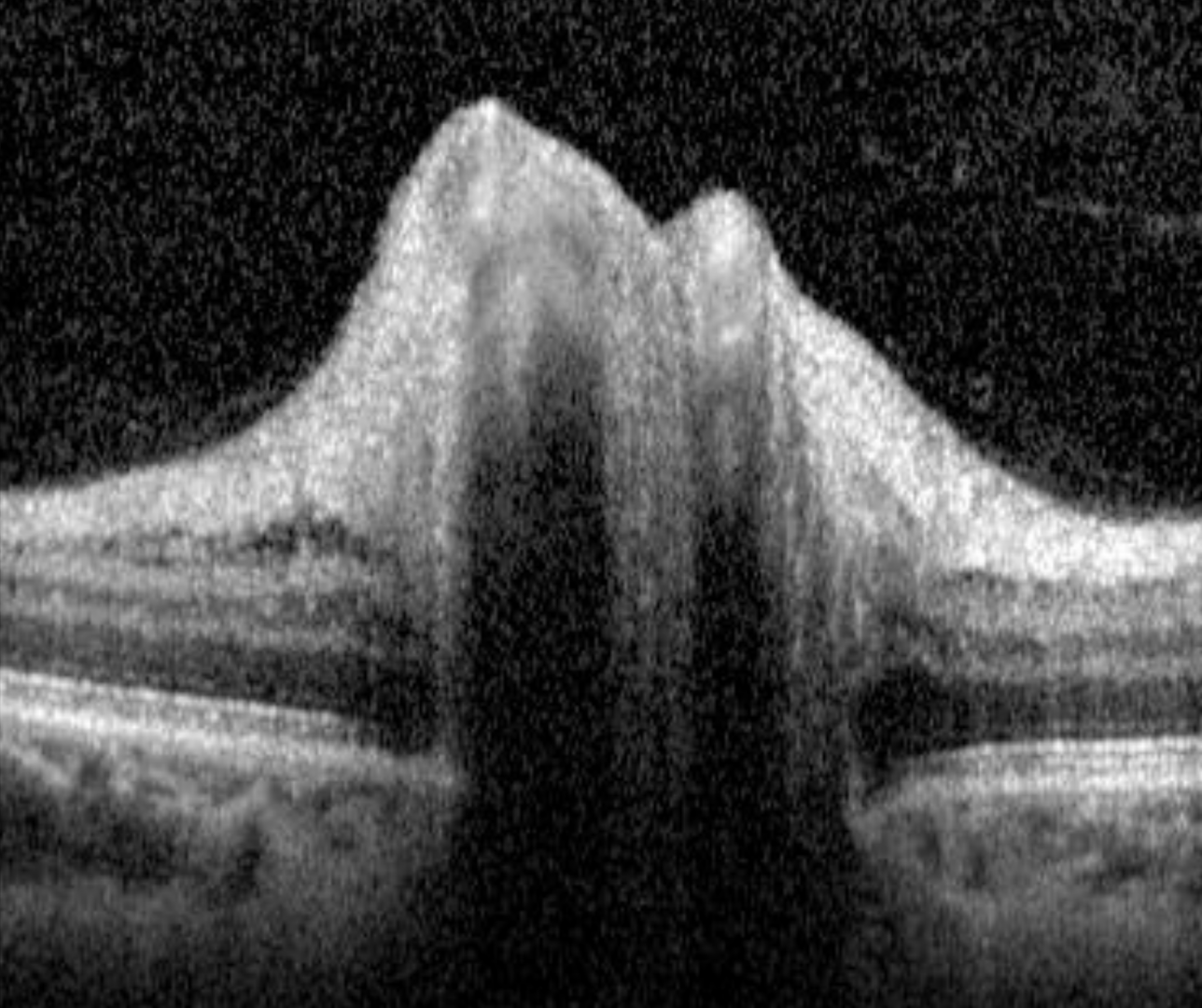
Diabetic papillopathy is a diagnosis of exclusion for patients with type 1 or type 2 diabetes who have disc oedema. It typically presents bilaterally with only a minimal disturbance to vision (if any) and a hyperaemic swelling of the optic nerve. A relative afferent pupillary defect is often not present and if it is, it is only mild. Mild vascular changes around the optic nerve head (as well as in the fundus) may be noted including venous engorgement with radially oriented disc telangiectasias and it may occur at any age in people with diabetes.
In contrast, non arteritic anterior ischaemic optic neuropathy is associated with more significant visual disturbance, an appreciable RAPD, and attenuated peripapillary vasculature. It typically occurs after the age of 50.
Treatment for diabetic papillopathy is typically not required as it is typically self-limiting, but still the patient still requires care within a collaborative team as it is a manifestation of systemic disease that can progress to more severe vision loss.
A diagnosis of diabetic papillopathy is reached only after other possible causes of optic nerve oedema are excluded, including raised intracranial pressure as well as other inflammatory, infective or infiltrative causes.
Differential diagnosis
References
Giuliari GP, Sadaka A, Chang PY, Cortez RT. (2011) Diabetic papillopathy: current and new treatment options. Curr Diabetes Rev. May;7(3):171-5.
Slagle WS, Musick AN, Eckermann DR. (2009) Diabetic papillopathy and its relation to optic nerve ischemia. Optom Vis Sci. Apr;86(4):e395-403.