Overview
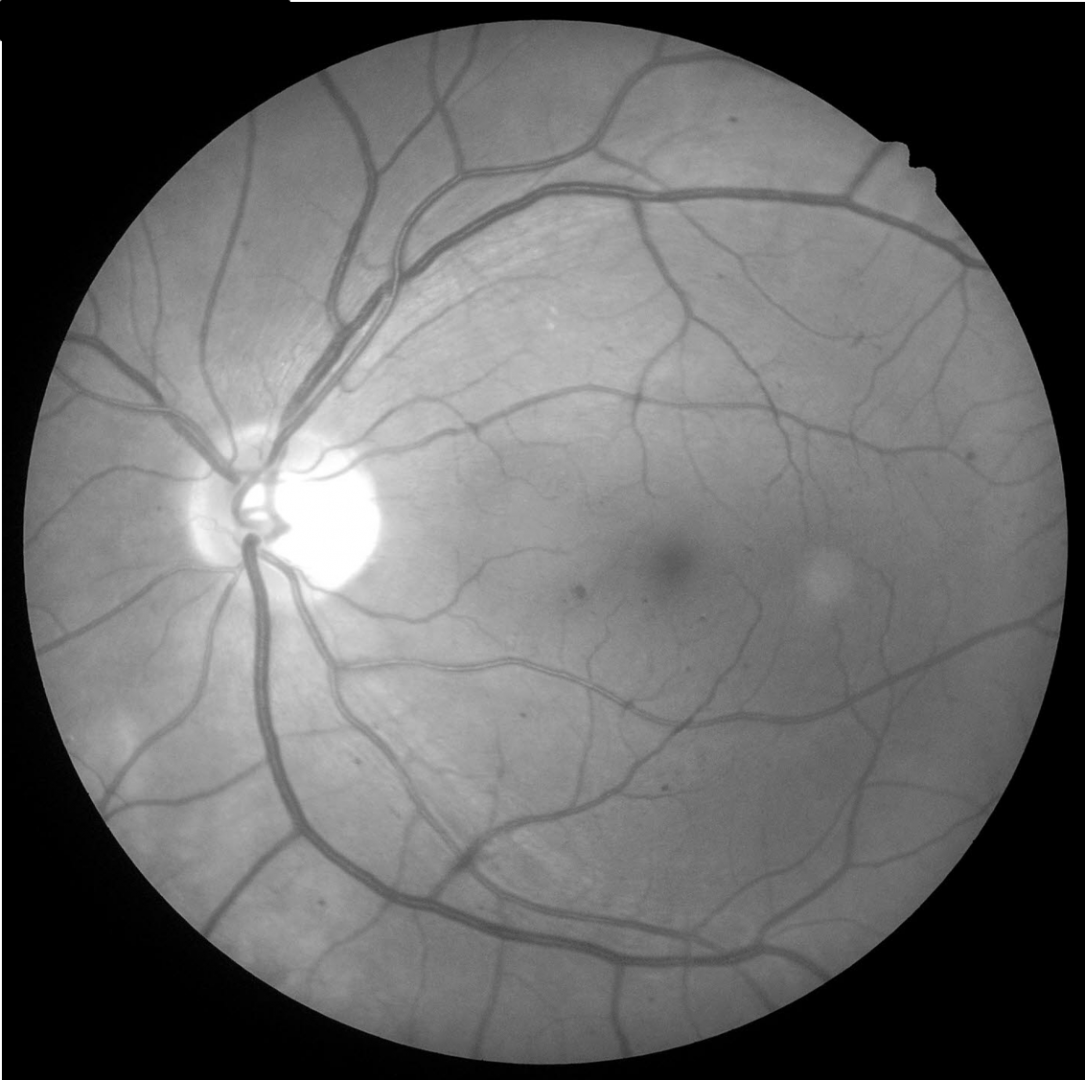
The term "non-proliferative diabetic retinopathy" (NPDR) is used when a patient with diabetes has funduscopic signs including one or more of the following lesions (in the absence of neovascularisation or pre-retinal/vitreous haemorrhage): microaneurysms, intraretinal (dot/blot/flame) haemorrhages, cotton wool spots, intraretinal microvascular abnormalities (IRMA) and/or venous beading.
Within this general classification, sub-classifications exist that reflect the relative severity of the retinal changes and correlate with the risk of vision loss.
Using the International Clinical Diabetic Retinopathy Severity Scale, the levels of NPDR are as follows:
- Mild NPDR: presence of microaneurysms only.
- Moderate NPDR: more changes than just microaneurysms, but the criteria for severe NPDR (below) is not met.
- Severe NPDR (4-2-1 rule): any of the following changes WITHOUT any signs of proliferative diabetic retinopathy:
1. More than 20 intraretinal haemorrhages in each of the four quadrants
2. Definite venous beading in 2 or more quadrants
3. Prominent IRMA in 1 or more quadrant
It is important to note that macular oedema may be present at any stage of diabetic retinopathy, from mild NPDR through to PDR. The grading of macular oedema is discussed in further detail elsewhere in this Atlas (please click the link at the bottom of this page).
Some examples of each stage of NPDR are below.
Case Examples
-
Case 1: Mild NPDR
A 72 year old Caucasian female with most recent HbA1c of 7%. She was diagnosed with type 2 diabetes 20 years previously. Her best corrected visual acuity in the right eye is 6/6 (20/20). This case will focus on the right eye only.
-
Case 2: Moderate NPDR
An 87-year-old Middle Eastern male who was diagnosed with type 2 diabetes 5 years previous. He does not know his HbA1c but reports that his diabetes is well controlled. He also has hypertension, controlled by medication. His best corrected visual acuity in the right eye is 6/15+1 (20/50+1). A posterior subcapsular cataract was noted in this eye.
-
Case 3: Moderate NPDR
A 44-year-old Caucasian male who was diagnosed with type 1 diabetes at the age of 18. He is unsure of his latest HbA1c.
Intraocular pressures were 14mmHg in both eyes and there was no evidence of iris or angle neovascularisation. His best corrected visual acuity in the left eye is 6/9.5 (20/30). This case will focus on the left eye only. -
Case 4: Severe NPDR
A 57 year old Caucasian male with best corrected visual acuity of 6/6 (20/20) in the right eye and proliferative diabetic retinopathy in the left. His most recent HbA1c was reportedly "high". He also has systemic hypertension that is controlled with medication.
Differential Diagnosis
References
Alam, M, Zhang, Y, Lim, JI, Chan, R. Yang, M, Yao, X, (2020) Quantative optical coherence tomorgraphy angiography features for objective classification and staging of diabetic retinopathy. Retina: February 2020 - Volume 40 - Issue 2 - p 322-332
Duh, E. J., Sun, J. K., & Stitt, A. W. (2017). Diabetic retinopathy: current understanding, mechanisms, and treatment strategies. JCI insight, 2(14).
Proposed international clinical diabetic retinopathy and diabetic macular edema disease severity scales. Ophthalmology, Volume 110, Issue 9 - p 1677-1682
Johannesen, SK., Viken, JN., Vergmann, AS. and Grauslund, J. (2019), Optical coherence tomography angiography and microvascular changes in diabetic retinopathy: a systematic review. Acta Ophthalmol, 97: 7-14.
Tran, K. Pakzad-Vaezi, K (2018) Multimodal imaging of diabetic retinopathy, Current Opinion in Ophthalmology: November - Volume