Overview
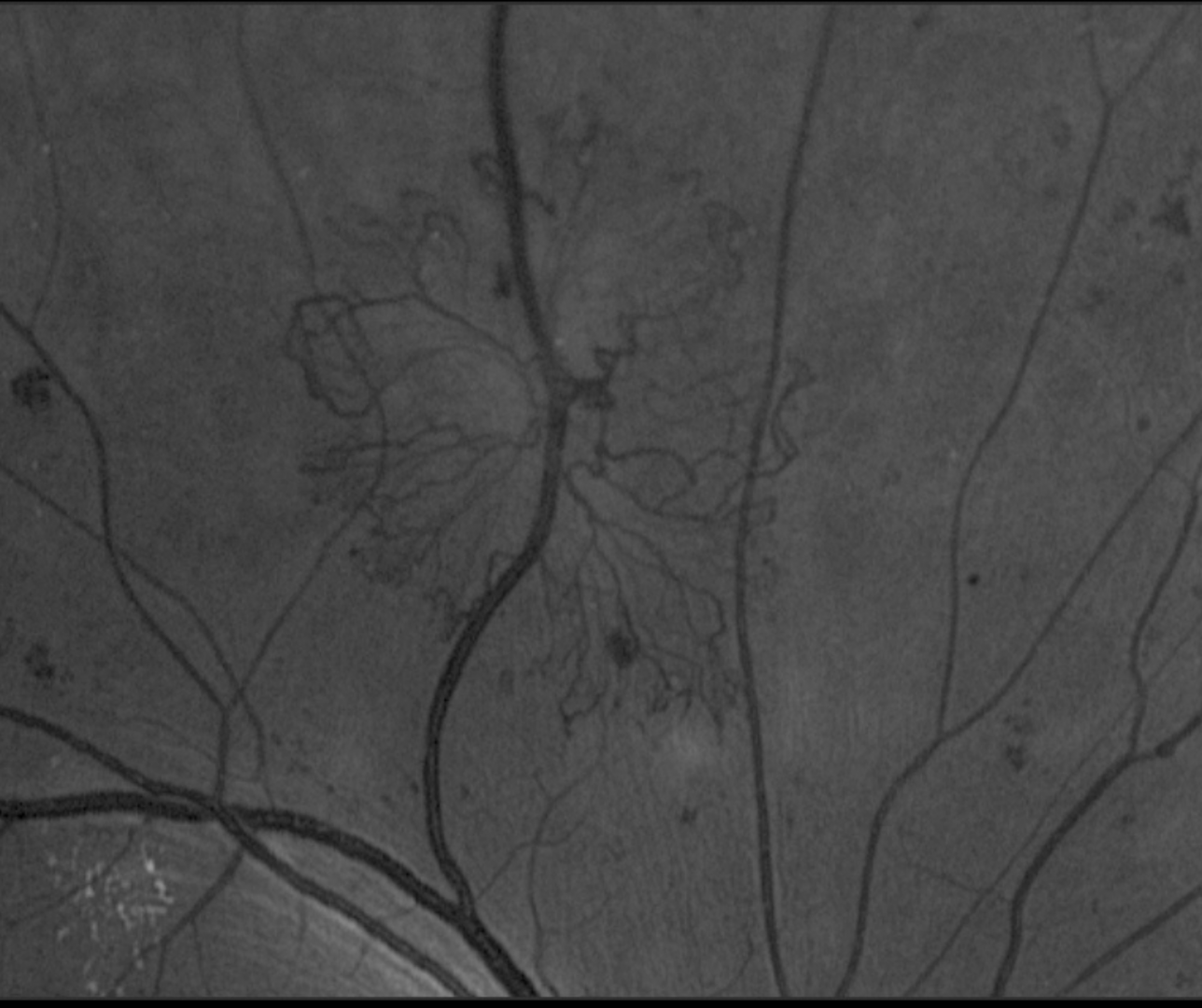
Proliferative diabetic retinopathy is defined by the presence of retinal neovascularisation with our without associated pre-retinal or vitreous haemorrhage in a patient with diabetes and other characteristic signs of diabetic retinopathy. It results from chronic hyperglycaemia leading to a complex array of biochemical and angiogenic changes in the retinal tissues.
Retinal neovascularisation may result in significant vision loss through tractional retinal detachment, vitreous or pre-retinal haemorrhages and/or neovascular glaucoma. Following are a series of case examples of PDR.
Case Examples
-
Case 1: Neovascularisation Elsewhere (sea-fan formation)
A 34-year-old female with type 1 diabetes, diagnosed when she was 17 years old. She reports a history of poor glycaemic control that has been progressively improving in recent years. Her most recent HbA1c was 8.1% and she reports no numbness or tingling in her extremities. Her best corrected visual acuity in the left eye is 6/9.5 (20/30). This case will focus on the left eye only.
Fundus photograph and red-free image (right eye)
More infoFundus photograph and red-free image (superior retina, right eye)
More infoOptomap green separation image (right eye)
More infoOptomap and green separation widefield images (superior retina, left eye)
More infoPosterior pole photo and red-free image montage (left eye)
More infoOptomap green separation image (left eye)
More infoSpectralis OCT line scans (right eye)
More infoSpectralis OCT Volume scan (left eye, supero-temporal retina)
More infoCirrus OCT Angiography (right eye)
More infoCirrus OCT Angiography (left eye)
More info -
Case 2: Proliferative diabetic retinopathy with NVD, NVE and vitreous haemorrhage
A 43-year-old Caucasian male diagnosed with type 2 diabetes 15 years previous. He reports a history of poor blood glucose control with a past HbA1c of 13%. More recently his diabetes has been better managed and his HbA1c has improved to 8%. 12 months ago he underwent an amputation of several toes due to complications from his diabetic neuropathy. He also reports poor renal function associated with his diabetes.
He notes that his vision on the day of this examination is worse than usual. His best corrected visual acuity is found to be 6/24 (20/80) in his right eye. This case will focus on the right eye only.
Funuds photograph (right eye)
More infoRed-free image (right eye)
More infoOptomap and green separation image (right eye)
More infoSpectralis OCT volume and line scans (right optic disc)
More infoMagnified view of vitreous and pre-retinal haemorrhages
More infoSpectralis OCT volume and line scans through vitreous and pre-retinal haemorrhages
More infoSpectralis OCT line scan (focal retinal traction)
More infoSpectralis OCT line scan (right macula)
More info -
Case 3: Neovascularisation and development of pre-retinal haemorrhage (PRH)
A 60-year-old Caucasian male with poorly controlled diabetes and latest HbA1c of 11.4%. At his initial visit, his best corrected visual acuity was 6/7.5 (20/25) in the left eye. The right eye has had pan-retinal laser photocoagulation due to extensive proliferative changes and tractional retinal detachment.
-
Case 4: Wolf's jaw configuration
A 60-year-old Caucasian male with type 2 diabetes, diagnosed 15 years previously, and systemic hypertension. He has previously had foot amputation due to diabetes-related complications. He reports his most recent HbA1c was 8%. His best corrected visual acuity in the left eye is 6/9.5-1 (20/30-1). This case will focus on the left eye only. Grade 2 nuclear sclerosis was identified in this eye.
-
Case 5: Neovascularisation of the disc
A 47-year-old Middle Eastern female who was diagnosed with type 2 diabetes 15 years previously. Her most recent blood glucose level was 12.0 mmol/L (216 mg/dl) and she is unsure of her HbA1c. Her best corrected visual acuity in the left eye is 6/30 (20/100). This case will focus on the left eye only.
Fundus photography and red-free image (left eye)
More infoOptomap and green separation image (left eye)
More infoOptic disc images (Optomap and green separation - left eye)
More infoSpectralis OCT line scan (left optic disc)
More infoCirrus OCT Angiography 4.5 x 4.5mm (left optic disc)
More infoCirrus OCT Angiography 12 x 12mm (left eye)
More info -
Case 6: Proliferative diabetic retinopathy with laser treatment
A 58-year-old Caucasian male with type 1 diabetes, diagnosed 45 years previously. His most recent HbA1c is 8.0% and his best corrected visual acuity in the left eye is 6/9-1 (20/30-1). He has previously had previous pan-retinal laser photocoagulation. This case will focus on the left eye only.
Differential Diagnosis
References
Alam, M, Zhang, Y, Lim, JI, Chan, R. Yang, M, Yao, X, (2020) Quantative optical coherence tomorgraphy angiography features for objective classification and staging of diabetic retinopathy. Retina: February 2020 - Volume 40 - Issue 2 - p 322-332.
Duh, E. J., Sun, J. K., & Stitt, A. W. (2017). Diabetic retinopathy: current understanding, mechanisms, and treatment strategies. JCI insight, 2(14).
Proposed international clinical diabetic retinopathy and diabetic macular edema disease severity scales. Ophthalmology, Volume 110, Issue 9 - p 1677-1682
Johannesen, SK., Viken, JN., Vergmann, AS. and Grauslund, J. (2019), Optical coherence tomography angiography and microvascular changes in diabetic retinopathy: a systematic review. Acta Ophthalmol, 97: 7-14.
Tran, K. Pakzad-Vaezi, K (2018) Multimodal imaging of diabetic retinopathy, Current Opinion in Ophthalmology: November - Volume 29 - Issue 6 - p 566-575