Overview
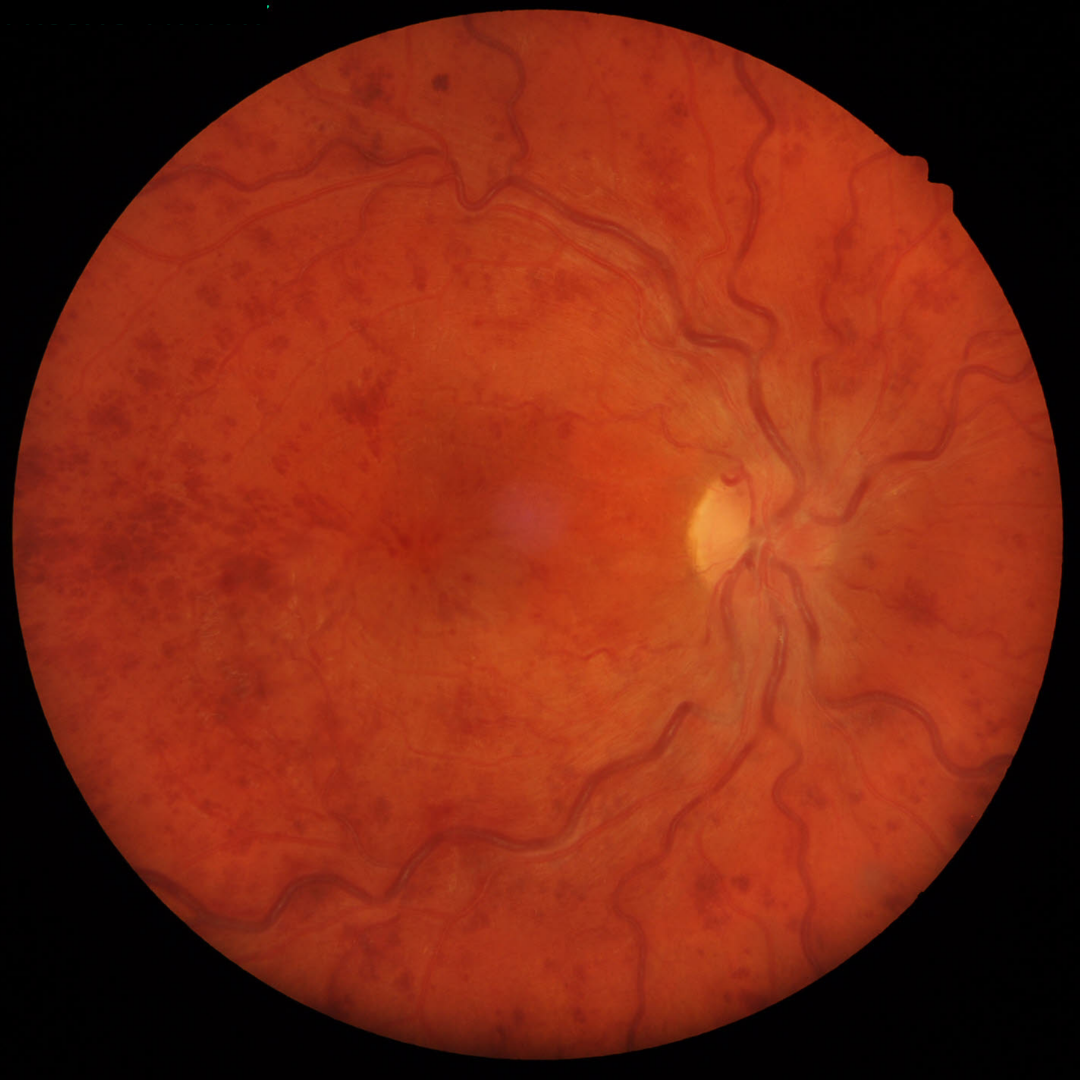
Central retinal vein occlusion represents an occlusion to the central vein. Its retinal presentation may be variable from mild to severe, the later often described as "blood and thunder" fundus.
Hallmark signs include retinal hemorrhages, which may extend peripherally, venous dilatation and tortuosity frequently in four quadrants as well as varying degrees of retinal / disc oedema and cotton wool spots. The severity of the occlusion will be reflected by the extent and presence of most / all of these signs.
Patients may be asymptomatic or experience significant visual disability depending on the extent of the retinal hemorrhages, cystoid macula oedema and or ischemia.
In highly ischemic cases there is a risk for neovascularization of the iris / angle and subsequent glaucoma.
Chronic cases of CRVO may lead to the development of collateral vessels which act to reroute blood from an obstructed vein to one that is unobstructed. These collateral vessels are typically found within the optic disc or adjacent retina in a CRVO. Clinically, they have a tortuous appearance and can be difficult to distinguish from retinal (or disc) neovascaulrisation without OCT imaging.
Collateral vessels are found in the deep vascular complex (intra-retinal location) while retinal neovascularisation is found on the retinal surface and posterior hyaloid interface.
Caes Examples
-
Case 1: Recent CRVO
A 70 year old Caucasian male with best corrected visual acuity of 6/24 (20/80) in the right eye. He experienced a reduction in the vision of his right eye 3 weeks previously, since which he has been under the care of an ophthalmologist for a CRVO in his right eye. He is a previous smoker, has a history of chemotherapy treatment for cancer and is currently also being treated for glaucoma in both eyes.
-
Case 2: Acute CRVO
A 72 year old Asian male with best corrected visual acuity of 6/15+2 (20/50+2) in the left eye.
-
Case 3: Acute CRVO
A 72 year old Middle Eastern male who takes medication for elevated blood pressure. Visual acuity in his right eye is 6/12 (20/40), reduced from 6/6 (20/20) at his appointment 6 months prior.
-
Case 4: Acute CRVO
A 30 year old Caucasian male with best corrected visual acuity of 6/6 (20/20) in the right eye. Ocular history is remarkable for a previous branch retinal vein occlusion in the superior right macula about 12 months earlier. He went to see his optometrist for a routine eye exam. He is taking Warfarin for a genetic condition.
Fundus photograph (right eye)
More infoStereoscopic disc photo
More infoGreen separation images (acute presentation)
More infoOptomap images - initial and follow-up visits
More infoGreen separation image (follow-up visit)
More infoSpectralis OCT volume scans (right macula)
More infoSpectralis OCT line scans (right optic nerve)
More infoCirrus RNFL analysis (initial and 12 month follow-up)
More info -
Case 5: Resolving CRVO
A 47 year old Asian male reported being diagnosed with a CRVO in the left eye, 9 months prior. Medical history was remarkable for genetic blood clotting disorder.
-
Case 6: Development of collateral vessels
A 39 year old Middle Eastern male complaining of reduction in the vision of his right eye for the last 5 days. Best corrected visual acuity in the right eye was 6/12 (20/40)
This case shows images from the initial visit where an acute CRVO was diagnosed and ophthalmology referral provided. It also includes a follow-up visit 2 months later following 2 Eylea injections.
-
Case 7: Previous CRVO with collateral vessels
A 73 year old Caucasian female, recently diagnosed with type 2 diabetes and hypertension, both of which were controlled with medication, having quit smoking 4 months prior. She reports no significant ocular history and had BCVA of 6/6 (20/20) in each eye.
Differential Diagnosis
References
Jia Li, Yannis M. Paulus, Yuanlu Shuai, Wangyi Fang, Qinghuai Liu, and Songtao Yuan (2017) New Developments in the Classification, Pathogenesis, Risk Factors, Natural History, and Treatment of Branch Retinal Vein Occlusion. Journal of Ophthalmology Volume 2017 |Article ID 4936924.
Khayat, Survey Ophth 2018. Major Review: Ischemic retinal vein occlusion: characterising the more severe spectrum of retinal vein occlusion
Patel, A., Nguyen, C., & Lu, S. (2016). Central Retinal Vein Occlusion: A Review of Current Evidence-based Treatment Options. Middle East African journal of ophthalmology, 23(1), 44–48.
Williamson, TH (1997) Central retinal vein occlusion: what’s the story? British Journal of Ophthalmology 81:698-704.
Woo SCY , Eye 2016. Associations of RAO and RVO to mortality, stroke and myocardial infarction: a systematic review