Overview
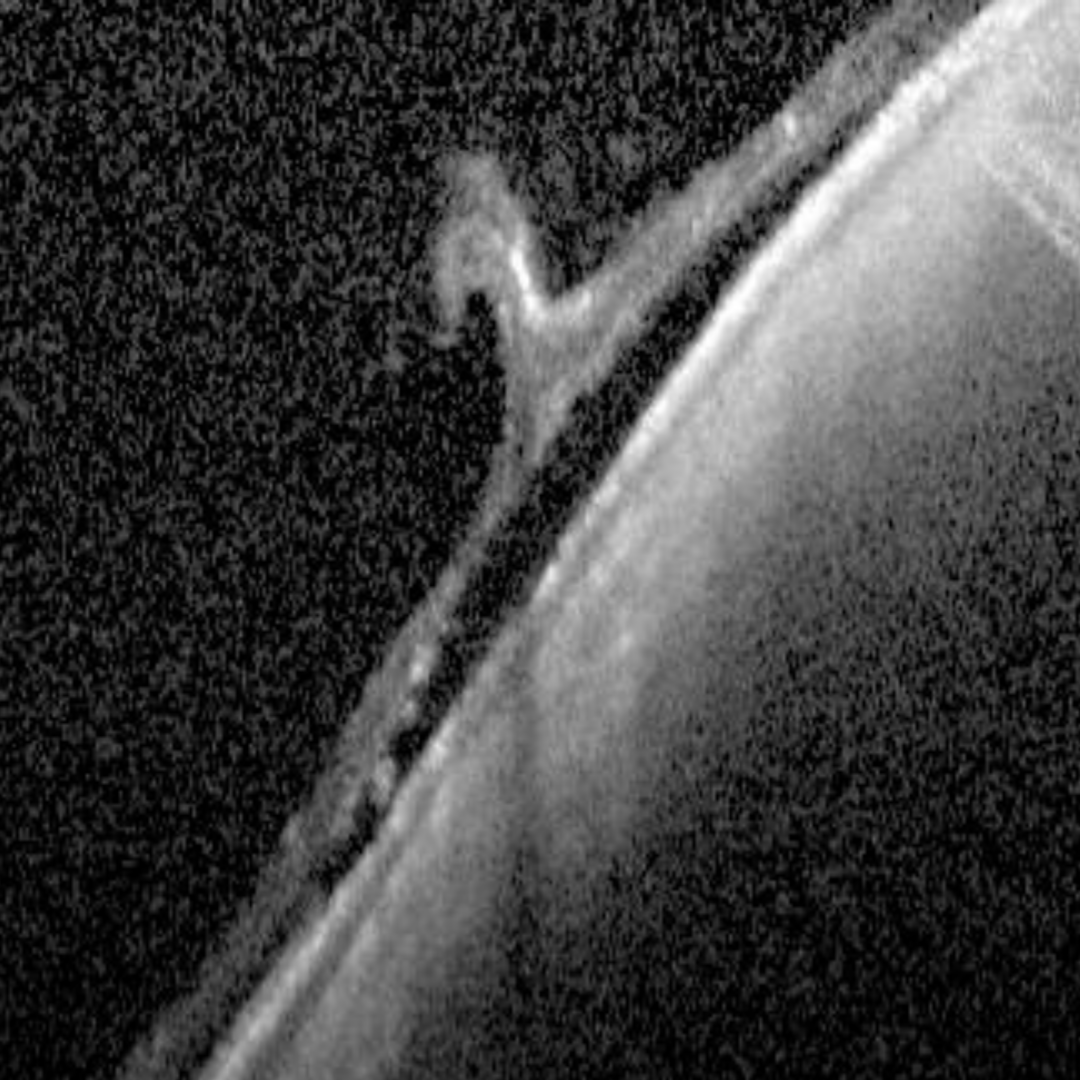
A vitreoretinal tuft is characterised by an area of abnormal vitreoretinal attachment. Associated vitreoretinal traction may be associated with retinal breaks and/or sub-clinical retinal detachment.
There are 2 main types of vitreoretinal tufts.
Non-cystic tufts are found in up to 72% of adults, usually in the far peripheral retina. They are short, thin projections of abnormal retinal and glial tissue less than 0.1mm in diameter. The tips of non-cystic tufts may break off causing floaters in the vitreous, however this type of cyst does not lead to the formation of retinal holes or tears.
Cystic tufts appear as round-shaped grey-white nodules on retinal examination and widefield imaging, and are usually equatorial in location. They are often associated with RPE hyperplasia and are larger than 0.1mm.
OCT imaging of cystic vitreoretinal tufts reveals the presence of internal microcysts. A posterior vitreous detachment (PVD) can cause increased traction at the location of the tuft, potentially resulting in a retinal tear, operculated hole or retinal detachment.
Retinal tufts have been identified as the cause of approximately 1% of rhegmatogenous retinal detachments. This low level of risk means that prophylactic treatment of cystic retinal tufts remains controversial.
Case Examples
-
Case 1
A 51-year-old Caucasian male with best corrected visual acuity of 6/4.8 (20/15) in the right eye.
Optomap pseudocolour and green separation image (right temporal retina)
More infoSpectralis OCT vertical line scan through the anterior tuft
More infoSpectralis OCT line scan of the more anterior tuft
More infoSpectralis OCT line scan through the more posterior tuft
More infoSpectralis OCT volume scan through the vitreoretinal tufts
More info -
Case 2
An asymptomatic 21-year-old Asian male with high myopia (-12.00DS) in the left eye, and best corrected visual acuity of 6/7.5 (20/25) in this eye.
-
Case 3
A 40-year-old Caucasian female with moderate myopia (-5.00DS) in the right eye and best corrected visual acuity of 6/7.5 (20/25) in this eye.
-
Case 4
A 48-year-old asymptomatic Caucasian male with best corrected visual acuity of 6/4.8 (20/15) in the left eye.
Differential Diagnosis
References
Lewis, H (2003) Peripheral retinal degenerations and the risk of retinal detachment, American Journal of Ophthalmology, Volume 136, Issue 1, pages 155-160,
Shaimov R.B., Shaimova V.A. (2017) Vitreoretinal Degenerations. In: Shaimova V. (eds) Peripheral Retinal Degenerations. Springer, Cham.