Overview
Toxoplasmosis is a focal, necrotising chorioretinitis caused by the parasite Toxoplasma gondii. This parasite may be ingested by eating undercooked meat contaminated with tissue cysts or oocysts, and may also be transmitted across the placenta to a foetus. 80% of lesions are visible soon after birth.
When inactive, a chorioretinal scar is seen. Recurrences of choioretinitis may occur in 2 of every 3 patients at some point in life, manifesting as new areas of white inflammation at the border of a chorioretinal scar. When active, this condition may be accompanied by systemic symptoms such as fever, malaise and lymphadenopathy.
Recurrences of retinochoroiditis can occur in up to two thirds of patients at some point later in life.
In immunocompromised patients, extensive retinal necrosis (often bilateral) may occur, potentially progressing to panuveitis.
OCT typically shows increased intraretinal reflectivity in areas of active retinitis. Posterior shadowing of the choroidal tissue and disorganisation of the retinal layers is also noted and there is often a thickening of the posterior hyaloid interface.
Chorioretinal scars from toxoplasmosis may show excavation and a disorganisation or loss of the overlying retinal layers. RPE hyperplasia is typically present in long-standing lesions, manifesting on OCT as a highly reflective RPE.
Case Examples
-
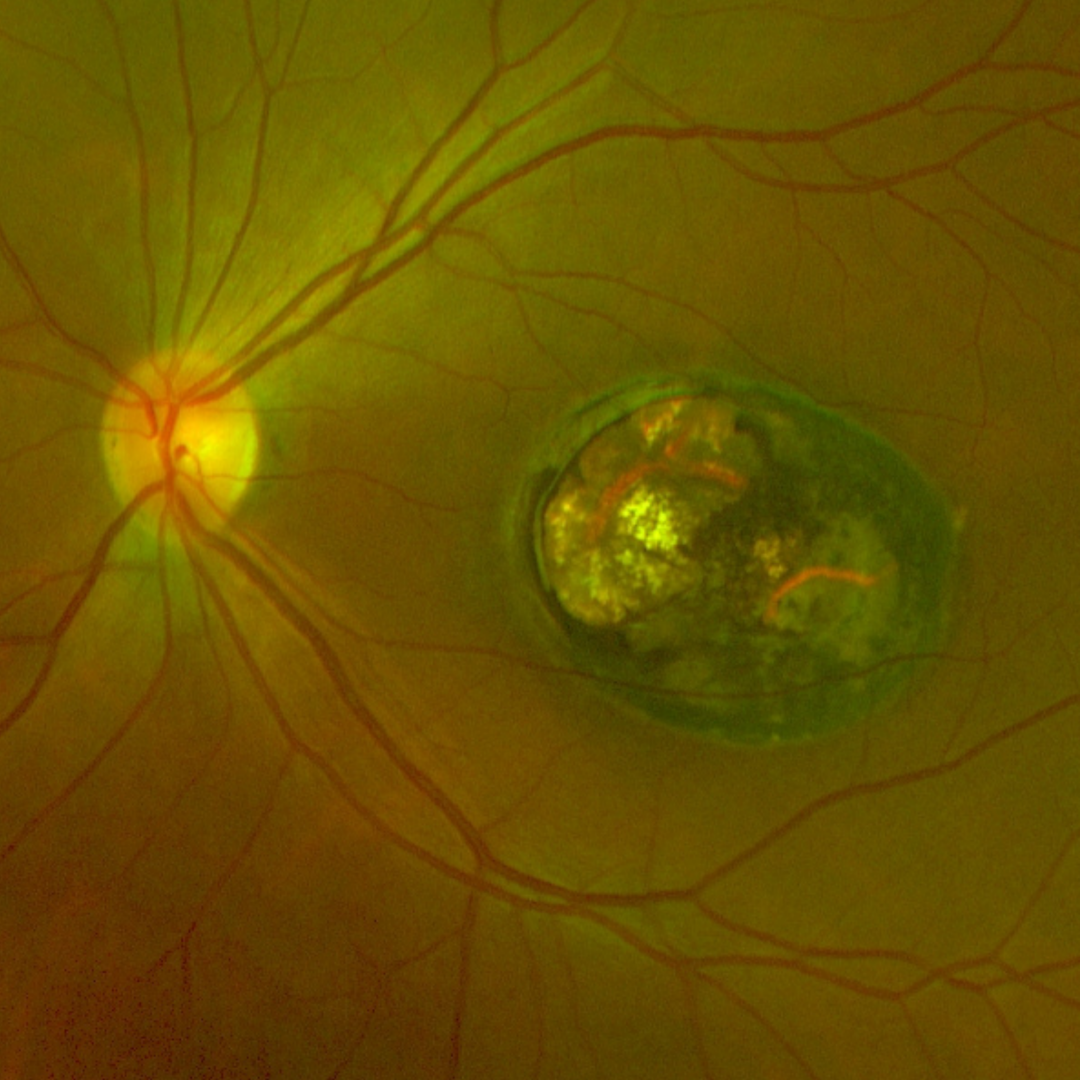
Case 1: Inactive toxoplasmosis scar at the macula
A 29 year old Asian female who reports poor vision in her left eye since she was very young. Her visual acuity in this eye is hand movements only.
-
Case 2: Inactive toxoplasmosis with fibrosis
A 35 year old Asian female with best corrected visual acuity in the left eye of 6/6- (20/20-). She was previously diagnosed with toxoplasmosis as a child.
Differential diagnosis
References
Brandão-de-Resende C, Balasundaram MB, Narain S, Mahendradas P, Vasconcelos-Santos DV (2020) Multimodal Imaging in Ocular Toxoplasmosis, Ocular Immunology and Inflammation, 28:8, 1196-1204