Overview
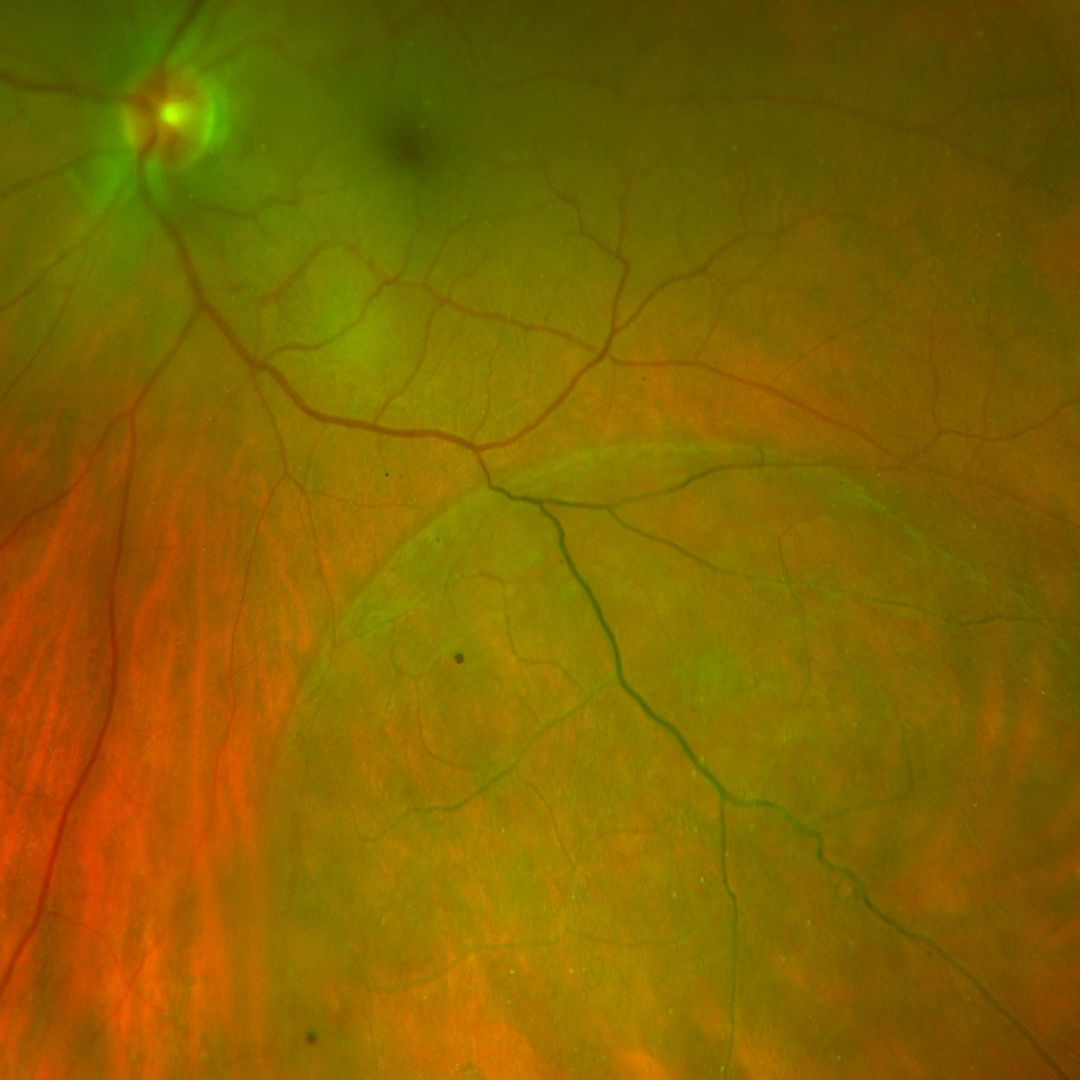
A bullous retinoschisis presents as an immobile dome-shaped elevation. The surface is smooth and transparent and lacks the folds typical of a retinal detachment. They may be associated with a reticular pattern of sheathed retinal vessels, isolated retinal haemorrhages and can be continuous with peripheral cystoid degeneration. Small whitish flecks can also be seen on its surface, called Gunn's dots.
OCT shows splitting of the retina anterior to the outer plexiform layer. The location of the split results in a thinner inner retinal layer than the typical (flat) type. Bullous retinoschisis is therefore more likely to develop breaks in the inner retina than the typical retinoschisis.
Most cases of retinoschisis are asymptomatic and non-progressive. However, it can progress to a retinal detachment if breaks occur in both the inner and outer “leaf”. In these cases, a break in the inner leaf allows liquified vitreous to enter the retina. A break in the outer leaf then allows this liquified vitreous to enter the subretinal space, causing separation of the RPE and neurosensory retina. In cases of a secondary retinal detachment, the presence of a pigmented demarcation line suggests chronicity.
Bullous retinoschisis should be examined routinely to check for progression to retinal detachment.
Case Examples
-
Case 1
A, asymptomatic 72 year old Caucasian male with best corrected visual acuity of 6/6- (20/20-) in the left eye.
-
Case 2
An asymptomatic 63 year old Middle Eastern male with best corrected visual acuity of 6/7.5 (20/25) in the left eye.
-
Case 3
An asymptomatic 44 year old Caucasian male with best corrected visual acuity of 6/6 (20/20) in his right eye.
-
Case 4
An asymptomatic 71 year old Caucasian male with best corrected visual acuity of 6/6- (20/20-)
Differential diagnosis
References
Hilel Lewis,Peripheral retinal degenerations and the risk of retinal detachment, American Journal of Ophthalmology, Volume 136, Issue 1,2003, Pages 155-160,
Thanos, A., Todorich, B., Pasadhika, S., Khundkar, T., Xu, D., Jain, A., Ung, C., Faia, L. J., Capone, A., Williams, G. A., Yonekawa, Y., Sarraf, D., & Wolfe, J. D. (2019). Degenerative Peripheral Retinoschisis: Observations From Ultra-Widefield Fundus Imaging. Ophthalmic Surgery, Lasers & Imaging Retina, 50(9), 557-564
Wallsh, JO, Gallemore,RP (2017) Identifying rhegmatogenous detachments in bullous retinoschisis with optical coherence tomography studies, American Journal of Ophthalmology Case Reports, Volume 6, Pages 38-40,