Overview
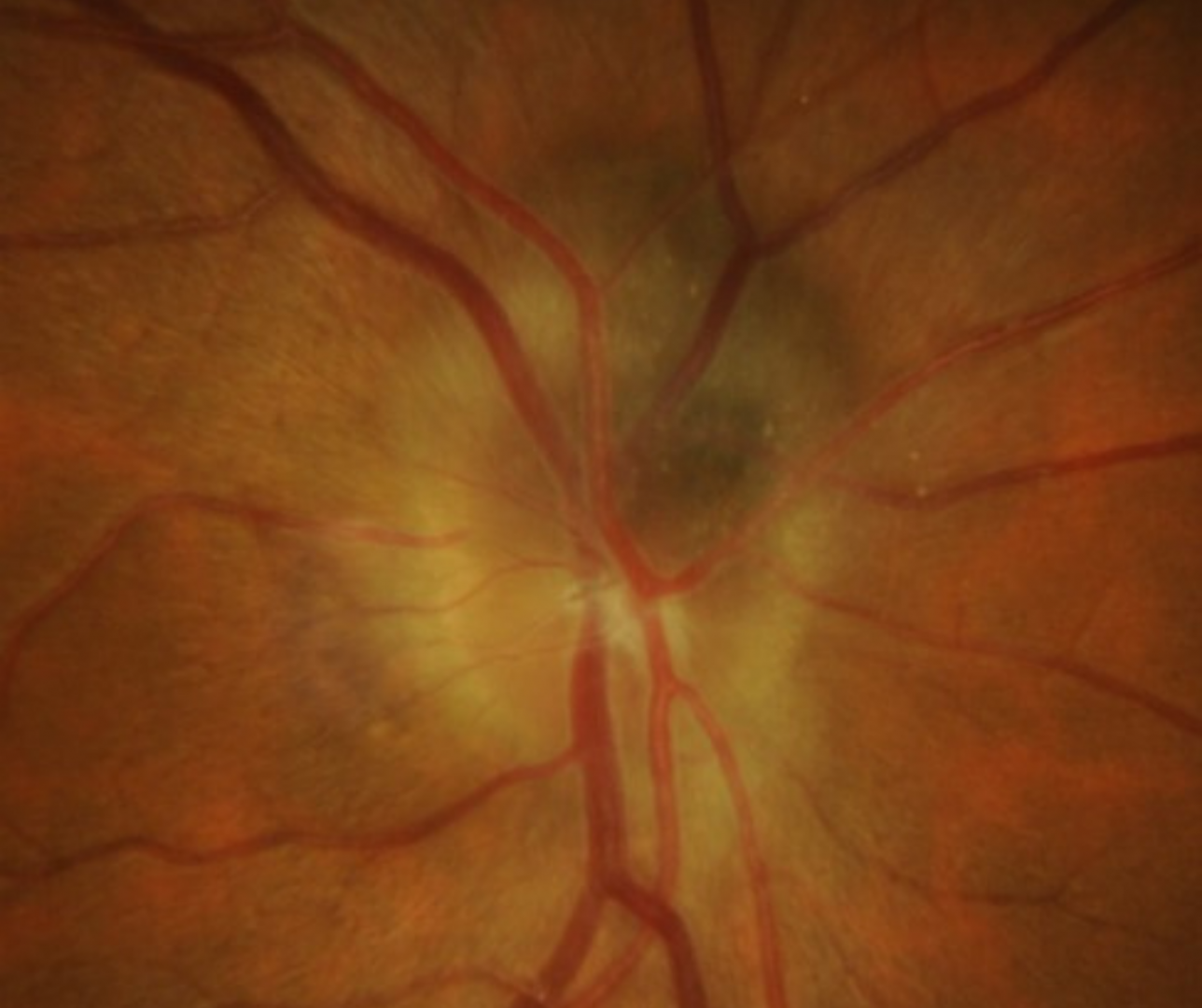
An optic nerve head (ONH) melanocytma is typically a benign pigmented tumour of melanocytes. It usually presents as an isolated entity with no systemic associations. Complications include optic disc oedema, intraretinal oedema, subretinal fluid, retinal haemorrhage and exudation. Malignant conversion occurs in 1-2% of cases.
Funduscopic features include a mildly elevated, dark-brown or black lesion on the optic disc that often extends into the peripapillary retina and choroid. It is typically small and unilateral.
When the choroid is involved, it resembles a juxtapapillary choroidal naevus whereas retinal involvement is usually black with a feathery margin.
OCT shows a nodular elevation with an irregular, hyper-reflective anterior border with posterior shadowing.
FAF shows a corresponding hypo-autofluorescence
Visual field defects occur in up to 90% of eyes, typically presenting as an enlarged blindspot, nasal step and arcuate defects.
B-scan ultrasound may show a small dome-shaped lesion or mild elevation at the optic nerve head with a high internal reflectivity.
Case Examples
-
Case 1
An asymptomatic 54 year old Caucasian female with best corrected visual acuity of 6/6 (20/20) in the right eye.
Fundus photograph (right eye)
More infoStereoscopic disc photo (right eye)
More infoOptomap (1), red separation (2) and green separation (3) images
More infoFundus autofluorescence image
More infoSpectralis OCT line scan through the lesion
More infoSpectralis OCT volume scan through the lesion
More infoB-Scan ultrasound (right eye)
More infoCirrus RNFL analysis
More info -
Case 2
An asymptomatic 36 year old Caucasian female with best corrected visual acuity of 6/7.5 (20/25) in the right eye.
Differential diagnosis
References
Gologorsky, D., Schefler, A. C., Ehlies, F. J., Raskauskas, P. A., Pina, Y., Williams Jr, B. K., & Murray, T. G. (2010). Clinical imaging and high-resolution ultrasonography in melanocytoma management. Clinical Ophthalmology (Auckland, NZ), 4, 855.
Mohmad, Z., Kah, T. A., Yong, K. C., Halim, W. H. W. A., & Yong, T. K. (2011). Melanocytoma of the optic nerve head-a diagnostic dilemma. Clinics and Practice, 1(3).
Parnes et al., 2011. The Evaluation and management of optic disc melanocytoma. AAO Eyenet Magazine.