Overview
Choroidal melanoma is the most common primary intraocular malignant tumor however in practice, it may be difficult to distinguish from a suspicious choroidal naevus. Please refer to the page "Choroidal naevus" in this resource for factors predictive of growth into melanoma (link provided at the bottom of this page).
Funduscopic features include a dome shaped lesion that may be associated with an exudative retinal detachment, orange pigment (lipofuscin), sentinel vessels, choroidal folds, subretinal fluid or haemorrhage. They are usually pigmented but can also mixed or amelanotic.
OCT EDI features include increased tumour thickness, subretinal fluid and overlying retinal disruptions including shaggy photoreceptors (irregular and elongation of the photoreceptors).
Autofluorescence imaging showed confluent areas of hyper-autofluorescence which correlates to the clinically orange pigment. The presence of subretinal fluid may also exhibit hyper-autofluorescence.
B-scan ultrasound shows an acoustically hollow lesion which may be dome or mushroom shaped.
Case Examples
-
Case 1
A 63 year old Caucasian male complaining of reduced vision in the left eye for the last few months. His best corrected visual acuity was 6/15 (20/50) in the left eye and testing with an Amsler grid revealed both central and nasal distortion.
Given the symptoms and clinical presentation, this patient was urgently referred to an ophthlamologist.
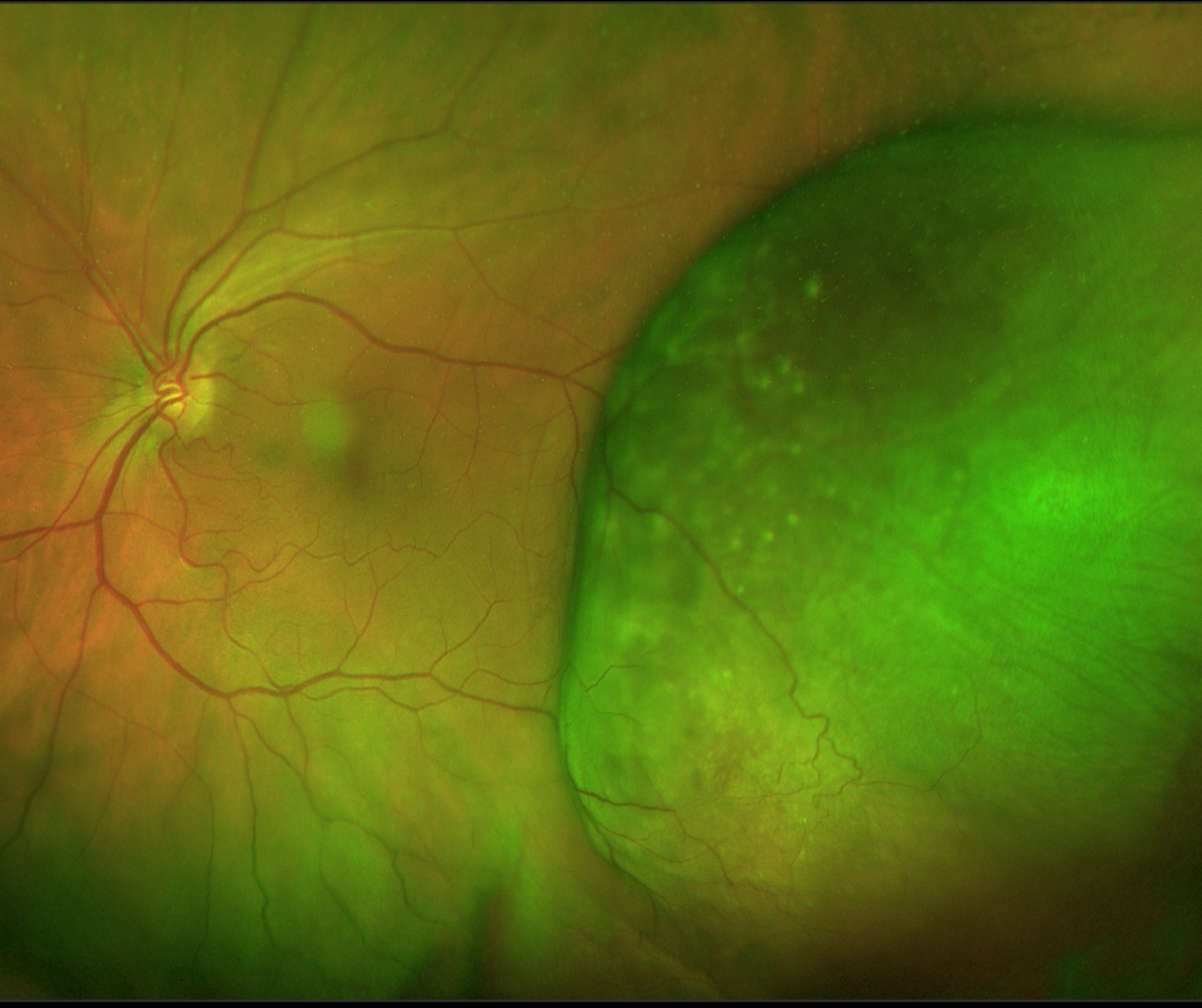
Optomap (1), green separation (2) and red separation (3) images - left eye
More infoFundus photograph (left temporal retina)
More infoSpectralis OCT lines through the lesion
More infoSpectralis OCT volume scan through the lesion
More infoCirrus OCT macular thickness map
More infoB-Scan ultrasound (left eye)
More info -
Case 2
A 61 year old Caucasian female complaining of a visual disturbance in the left eye. Best corrected visual acuity was 6/12- (20/40-) in this eye at initial presentation.
Central distortion of the vision in the left eye is noted on testing with an Amsler grid.
This patient was referred urgently to an ocular oncologist who diagnosed choroidal melanoma. The lesion was treated with transpupillary thermotherapy (TTT) which was repeated again one month later. The choroidal melanoma shrunk following the second treatment and regular review is now ongoing.
Optomap (1), red separation (2) and green separation (3) images - initial presentation
More infoSpectralis OCT line scan through lesion (at diagnosis)
More infoSpectralis OCT macular line scan (at diagnosis)
More infoOptomap (1), red separation (2) and green separation (3) images - 6 weeks post treatment
More infoOptomap (1), red separation (2) and green separation (3) images - 10 years post treatment
More infoOptomap images over time
More infoFundus autofluorescence images over time
More infoSpectralis OCT line scan at 5 year follow up
More info30-2 SITA Standard visual field
More info
Differential Diagnosis
References
Shields, CL. et al. (2012). Enhanced depth imaging optical coherence tomography of small choroidal melanoma: comparison with choroidal nevus. Archives of Ophthalmology, 130(7), 850-856.
Singh, P. et al. (2012). Choroidal melanoma. Oman journal of ophthalmology, 5(1), 3.