Overview
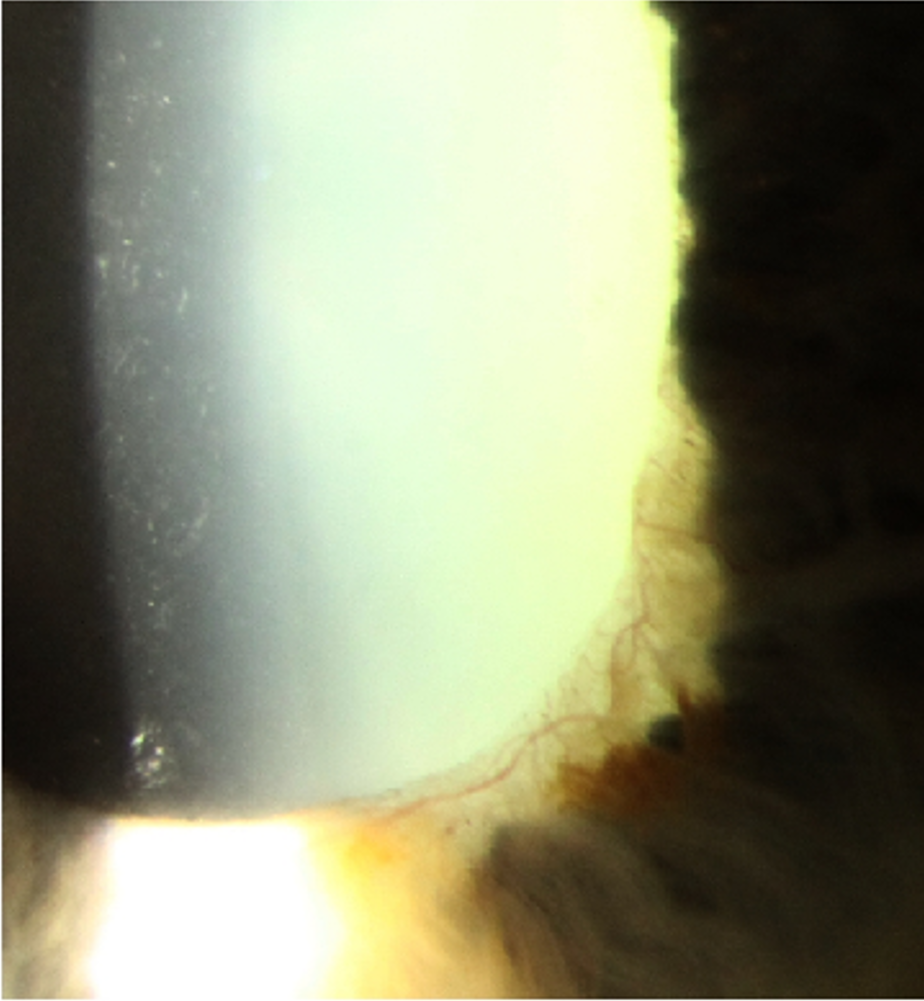
Neovascular glaucoma occurs as the result of neovascularisation of the iris and anterior chamber angle. The fibrous scaffolding that supports the neovascular network of vessels reduces aqueous outflow through the trabecular meshwork in the first instance. Over time this fibrous tissue contracts, causing synechial angle closure, resulting in high intraocular pressure.
Iris neovascularisation develops secondary to retinal ischaemia which triggers the release of vascular endothelial cell growth factor (VEGF). The most common causes of neovascular glaucoma are central vein retinal occlusion, proliferative diabetic retinopathy and ocular ischemic syndrome, central retinal artery obstruction, and links to each of these can be found at the bottom of this page.
Treatment is initially aimed at reducing intraocular pressure (medically or surgically) and undertaking pan retinal photocoagulation to prevent further release of VEGF. Recently the use of anti-VEGF injections has shown to be of benefit in treating neovascular glaucoma also.
Clinical Signs
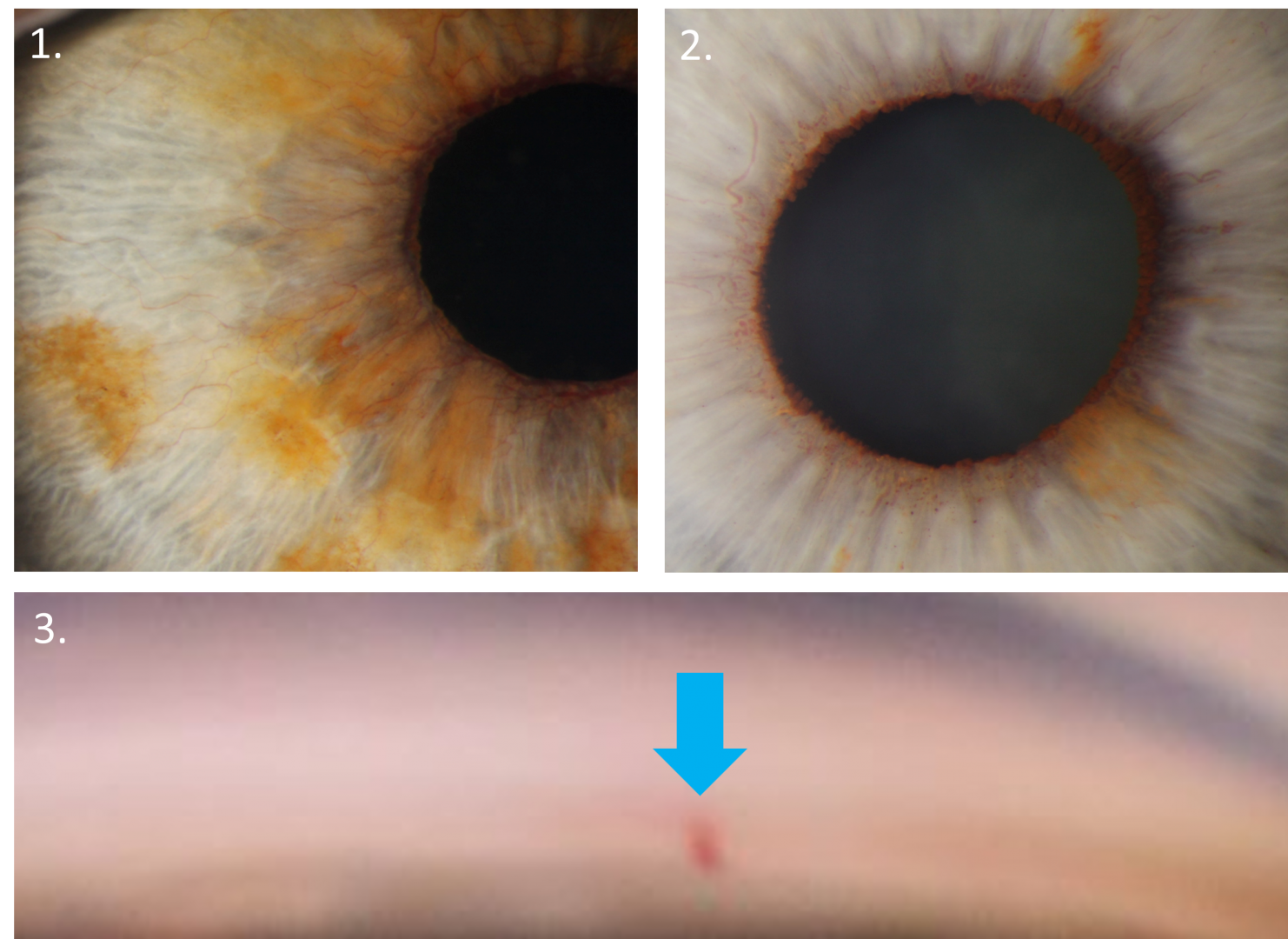
Slitlamp examination can reveal iris rubeosis (rubeosis irides)- fine vessels that do not follow a typical pattern of growth, unlike other iris vessels which are radially oriented (1). Rubeosis irides typically starts at the pupillary margin and is visible under high magnification as red spots (2)
Gonioscopy shows the presence of blood vessels in the angle. Over time, with disease progression, peripheral anterior synechiae can form and narrow the anterior chamber angle.
Case Examples
-
Case 1: End stage neovascular glaucoma
A 66 year old Middle Eastern female who has been "blind" in her right eye for several years. Vision in this eye is light perception only. The patient reports a history of central retinal vein occlusion approximately 10 years previous. Intraocuar pressure in the right eye was 39mmHg.
Fundus imaging was limited due to opaque media.
-
Case 2: Suspected neovascularisation of the angle
A 68 year old Caucasian male with poorly controlled type 2 diabetes. He is unsure of his HbA1c and his blood sugar level on the day of examination was 10mmol/litre. Intraocular pressures were 14mmHg OU in the context of average corneal thicknesses (555µm OD, 558µm OS).
-
Case 3: Iris neovascularisation
A 70 year old Caucasian male with type 2 diabetes and poor glycaemic control. Intraocular pressure in the left eye is 14mmHg in the context of average corneal thickness (pachymetry 545µm).
Associated Conditions
References
Rodrigues, GB., Abe, RY., Zangalli, C. et al. (2016) Neovascular glaucoma: a review. Int J Retin Vitr 2, 26.
Sun, Y. Liang, Y. Zhou, P. et al. (2016) Anti-VEGF treatment is the key strategy for neovascular glaucoma management in the short term. BMC Ophthalmol 16, 150.