Introduction
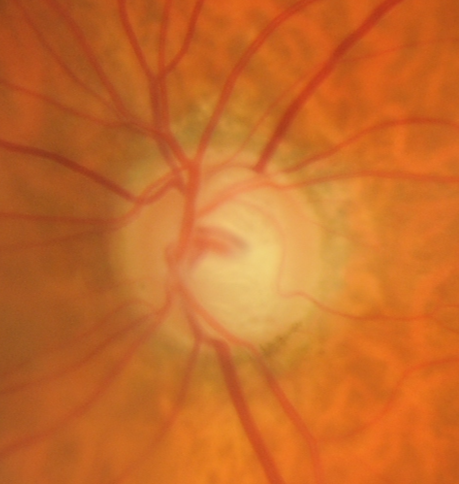
Here we will introduce a systematic approach to assessing the optic nerve head. Below we have identified the key features to note when conducting an optic disc assessment for glaucoma. It is considered best practice to address each of these features in your examination.
For your clinical assessment, disc appearance should be assessed using techniques that allow a stereoscopic view of the disc. This will allow you to appreciate the depth of cupping present, and more readily identify the edge of the cup (and any associated neuroretinal rim thinning).
Aspects of Disc Assessment
-
1. Disc Size
Disc size has significant impact on the size of the optic disc cup and rim thickness as we will outline later in this section. This makes it an important consideration in glaucoma diagnosis.
The simplest way to estimate disc size is to draw a line from the centre of the disc to the fovea, then estimate the length of this line in disc diameters (DD). If the discs are ellipsoid rather than round in shape, use the longest disc diameter in your estimation.
In an eye with an "average" sized disc, this distance is approximately 2.5DD.
In an eye with a "large" disc, this distance is less than 2.5DD
In an eye with a "small" disc, this distance is greater than 2.5DD
For the purposes of this estimation technique, the visible edge of the sclera is used to define the edge of the disc. From a histological perspective, the true edge of the disc may vary from this approximation, however it is close enough such that the accuracy of this estimation technique will not be affected.
Illustration of disc estimation technique in a patient with small discs
More infoIllustration of disc estimation technique in a patient with medium discs
More infoIllustration of disc estimation technique in a patient with large discs
More infoIllustration of disc estimation technique in a patient with an oval disc
More info -
2. Disc Shape
While many discs are regular in shape, rotation of the optic nerve head insertion and/or plane can cause the optic nerve to be oval or elliptical in shape.
These changes are referred to as either cyclotorsion (rotation of the disc around the anterior-posterior axis) or disc tilt (the plane of the disc is rotated around the longitudinal axis)
Cyclotorsion and disc tilt are typically seen in eyes with a long axial length or in tilted disc syndrome. Examples of each are provided.
-
3. Optic disc cup and the neuroretinal rim
Glaucoma is a progressive optic neuropathy that is associated with increased cupping, a loss of the neuroretinal rim and associated retinal nerve fibre layer (RNFL) thinning. For this reason, an analysis of optic disc cup and the neuroretinal rim is essential when assessing for glaucoma.
As discussed earlier, disc size is a important feature as it is a contributing factor to cup size. For example, a large cup is more concerning for glaucoma in a small disc compared to the large disc.
Historically, the cup:disc ratio was used to assess the optic nerve head, however this measure has several failings as it does not take into account the size of the disc, nor does it describe focal thinning of the neuroretinal rim which is an important marker of glaucoma.
Instead of using this ratio, our recommendation is to evaluate the neuroretinal rim, identifying areas of thinning or notching, and also to evaluate the cup in the context of disc size.
Neuroretinal rim loss indicates retinal ganglion cell axon loss so it is a crucial feature to note. A notch in the rim, for example is typically associated with an RNFL wedge defect and RNFL thinning on OCT analysis.
The NRR is typically thickest superiorly and inferiorly. It is recommended to assess the optic disc cup and neuroretinal rim stereoscopically as the rim colour on a 2-dimensional image is not necessarily indicative of the true edge of the cup. Stereopsis also provides a more accurate indication of the depth of the cup.
-
4. RNFL thinning
The retinal nerve fibre layer (RNFL) can be viewed as subtle striated reflections on the retinal surface. They are most easily visualised using a red-free filter although in very lightly pigmented fundi it may still difficult to see the RNFL striations.
Glaucoma is associated with a dropout of retinal axons which presents as a loss of the normal RNFL reflectivity, either focal or generalised. These areas of loss may be described as wedge defects or a generalised reduction and examples of each are provided below. Wedge defects are typically associated with focal rim thinning.
-
5. Disc Haemorrhages
A disc haemorrhage is defined as a superficial retinal haemorrhage in the RNFL layer, located no more than 1 disc diameter from the disc margin.
Disc haemorrhages are present in less than 10% of glaucomatous eyes and their presence may be associated with conditions other than glaucoma such as retinal vascular disease.
The haemorrhage itself does not cause problems and gets reabsorbed with time but there is evidence that focal rim/RNFL damage may follow a disc haemorrhage,(Akagi et al., 2018, Ophthalmol Glaucoma). Disc haemorrhages have been suggested to be a possible indicator of active damage or a predictor of progression.
The following images illustrate a wide range of disc haemorrhages.
Case 1: Two disc haemorrhages (right eye)
More infoCase 2: Temporal disc haemorrhage (right eye)
More infoCase 3: Large temporal disc haemorrhage (right eye)
More infoCase 4: Thin disc haemorrhage at 8 o'clock (right eye)
More infoCase 5: Small disc haemorrhage at 11 o'clock (left eye)
More infoCase 6: Inferior disc haemorrhage (right eye)
More info -
6. Peripapillary Atrophy
There are 3 types of peripapillary atrophy, each associated with a distinct clinical presentation and OCT characteristics.
1. Alpha PPA is associated with irregularities in the RPE and presents as irregular hyper- and hypo-pigmentation of the RPE. Alpha PPA is found further from the disc margin than beta or gamma PPA.
2. Beta PPA is defined as the visibility of the large choroidal vessels and scleral due to the loss the RPE and choriocapillaris.
3. Gamma PPA is characterised by the absence of Bruch's membrane. It is defined as the distance between the termination of the Bruch's membrane and the edge of the scleral canal (optic disc edge). It appears as a white crescent immediately adjacent to the edge of the optic disc.
Beta PPA, in particular, may be associated with localised RNFL damage. However, this may not be a specific indicator of damage, as a large proportion of the normal population (approx 40%) may have PPA (Lopes et al., 2014, BMC Ophthalmol).
The suggestion is that peripapillary atrophy should be evaluated in context of true glaucomatous structural changes.
References
Lopes, FS. Dorairaj, S. Junqueira, DL. et al. (2014) Analysis of neuroretinal rim distribution and vascular pattern in eyes with presumed large physiological cupping: a comparative study. BMC Ophthalmol 14, 72.
Spaeth GL. Henderer J. Liu C. Kesen M. Altangerel U. Bayer A. Katz LJ. Myers J. Rhee D. Steinmann W. (2002) The disc damage likelihood scale: reproducibility of a new method of estimating the amount of optic nerve damage caused by glaucoma. Trans Am Ophthalmol Soc. 2002;100:181-5; discussion 185-6.