Overview
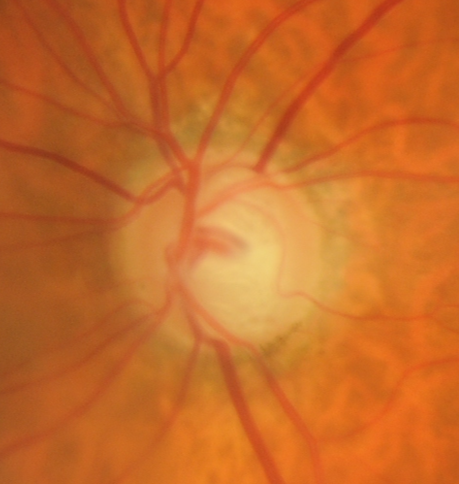
Primary open angle glaucoma (POAG) is characterised by elevated intraocular pressures (22mHg or higher), structural changes to the optic nerve head and retinal nerve fibre layer (RNFL) and/or visual field defects in the absence of secondary risk factors.
Normal tension glaucoma (NTG) exhibits the same clinical characteristics but without the measured IOP elevation. Normal tension glaucoma has been shown to be more prevalent in Chinese, Japanese, Korean, Indian and Singapore-Malay ethnicity (Cho et al., 2014). Among this group, incidence of NTG as a percentage of those with POAG has been reported to be as high as 92%.
Many systemic diseases/conditions are correlated with glaucoma, but are not causative. The strongest risk factors for glaucoma are age and family history, followed by myopia (for POAG). Other moderate risk factors for glaucoma include ocular trauma, migraine/vasospastic disorders, corticosteroid use and sleep apnoea. Hypertension and diabetes has been shown to be low risk factors.
The goal of glaucoma treatment is to reduce the intraocular pressure (IOP). Fluctuations in IOP (diurnal or across visits) are a strong risk factor for glaucoma progression (Sakata et al.) The ocular hypertension treatment study (OHTS) showed IOP lowering treatments to be effective in reducing structural and functional glaucomatous changes, and in lowering the rate of glaucoma suspects with high IOP converting to glaucoma. In normal tension glaucoma, although IOP is not elevated, treatment is aimed at reducing IOP by about 30% to minimise structural and/or functional progression.
POAG and Diabetes

POAG and diabetes share many common risk factors, and as noted above, diabetes is considered a low risk factor for the development of POAG. Recent research by Chauhan et al. (2024) found that (after accounting for other variables), development of diabetic retinopathy was higher among those patients with POAG (5.45%) than those without glaucoma (2.23%).
The potential clinical outcomes of this study are as follows:
• Patients might need to be assessed for DR more carefully or at closer intervals if they have they have concurrent POAG.
• Patients with POAG might require tighter control of glaucoma or may need to be treated earlier.
Glaucoma Assessment
References
Chauhan MZ, Elhusseiny AM, Kishor KS, Sanvicente CT, Ali AA, Sallam AB, Bhattacharya SK, Uwaydat SH, (2024) Association of Primary Open-Angle Glaucoma with Diabetic Retinopathy among Patients with Type 1 and Type 2 Diabetes: A Large Global Database Study,
Ophthalmology, https://doi.org/10.1016/j.ophtha.2024.01.016.
Kass MA, Heuer DK, Higginbotham EJ, et al. The Ocular Hypertension Treatment Study: A Randomized Trial Determines That Topical Ocular Hypotensive Medication Delays or Prevents the Onset of Primary Open-Angle Glaucoma. Arch Ophthalmol. 2002;120(6):701–713.
Hyun-kyung Cho, Changwon Kee (2014) Population-based glaucoma prevalence studies in Asians, Survey of Ophthalmology, Volume 59, Issue 4,
2014, Pages 434-447
McMonnies CW. (2017) Glaucoma history and risk factors. J Optom. 2017;10(2):71-78. doi:10.1016
Sakata R., Aihara M., Murata H. Intraocular pressure changes over a habitual 24-hour period, after changing posture or drinking water and related factors in normal tension glaucoma. Invest Ophthalmol Vis Sci. 2013;54:5313–5320