- Outline
- Case Examples
- Differential Diagnosis (Patchy CRA)
- Differential Diagnosis (Diffuse CRA)
- Related Topics
- References
Outline
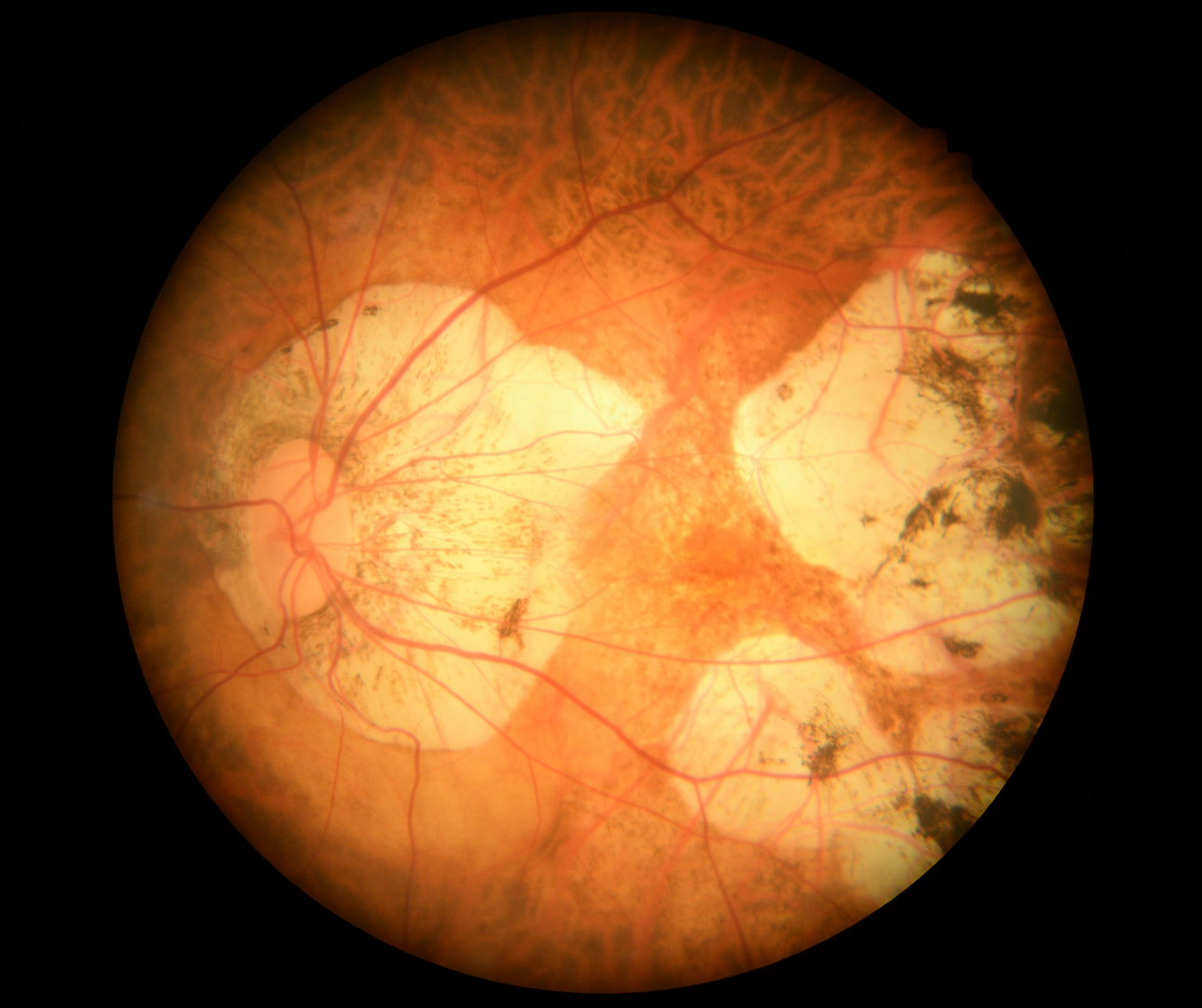
Chorioretinal atrophy (CRA) is associated with myopic maculopathy and prevalence tends to increase with age and axial length. There are typically two types of CRA described in the literature - patchy and diffuse.
Both types of CRA are associated with a risk of developing choroidal neovascularisation (CNV).
Patchy CRA can be classified into 3 types; it can develop from lacquer cracks, it can developed within an area of diffuse chorioretinal atrophy or it can form at the border of the posterior staphyloma. (Ohno-Matsui et al., 2018) .
Diffuse CRA is characterised by a yellowish white appearance at the posterior pole, varying from a small area adjacent to the optic disc and macula through to presentations that affect the entire posterior pole. On OCT significant thinning of the choroid is seen, typically with sporadic large choroidal vessels remaining
Patchy CRA is characterised by well-defined, white-grey lobules in the posterior pole that can enlarge over time. It presents as focal patchy areas of chorioretinal atrophy. Due to the absence of RPE and most of the choroid, the underlying sclera can be visualized. Large choroidal vessels may course through the atrophic region. OCT imaging through the areas of atrophy shows loss of the RPE, outer retina and most of the choroid.
Case Examples
-
Case 1: Diffuse Chorioretinal Atrophy
A 64 year old Asian female. Best corrected vision in the right eye is 6/75 (20/250) and the eye was reported to be amblyopic by her referring optometrist.
-
Case 2: Diffuse chorioretinal atrophy
A 68 year old Asian female with refraction -17.50 / -3.00 x 87 and visual acuity 6/18 (20/60).
-
Case 3: Patchy Chorioretinal Atrophy
A 64 year old Asian female. Refraction in the right eye was -3.50 / -5.75 x 75 VA 6/12- (20/40-).
-
Case 4: Patchy Chorioretinal Atrophy
A 43 year old Asian male with refraction in the left eye -7.00 /-1.00 x 85 and visual acuity of 6/7.5- (20/25-).
-
Case 5: Patchy chorioretinal atrophy
A 59 year old Asian male with refraction as follows:
Right eye: -16.00 / -2.75 x 170 VA 6/12 (20/40)
Left eye: -17.75 / -2.25 x 25 VA 6/9.5 (20/32) -
Case 6: Patchy chorioretinal atrophy
A 66 year old Asian female with high myopia. She has a posterior subcapsular cataract in the left eye and best corrected visual acuity is 6/9.5- (20/32-).
Differential Diagnosis (Patchy CRA)
Differential Diagnosis (Diffuse CRA)
References
Ng, D., Cheung, C., Luk, F. et al. (2016) Advances of optical coherence tomography in myopia and pathologic myopia. Eye 30, 901–916
Yasushi, I. (2017) Overview of the complications of high myopia, Retina: Volume 37 - Issue 12 - p 2347-2351
Ohno-Matsui, K., Ikuno, Y., Lai, TTI., Cheung, CMG (2018) Diagnosis and treatment guideline for myopic choroidal neovascularization due to pathologic myopia. Progress in Retinal and Eye Research, Volume 63, Pages 92-106,