Overview
Long-standing CSCR causes atrophy of the RPE and outer retina and may be associated with the development of choroidal neovascularisation. The changes associated with chronic CSCR are most evident on fundus autofluorescence imaging and OCT, as outlined below.
Chronic CSCR is considered to be active in the presence of sub-retinal fluid. If sub-retinal fluid is absent, it is considered to be inactive.
Chronic CSCR shows widespread RPE disruption and atrophy on OCT. Sub-retinal fluid may be present (active) or absent (inactive).
Fundus photography shows mottled pigmentary changes associated with the atrophic changes seen on OCT.
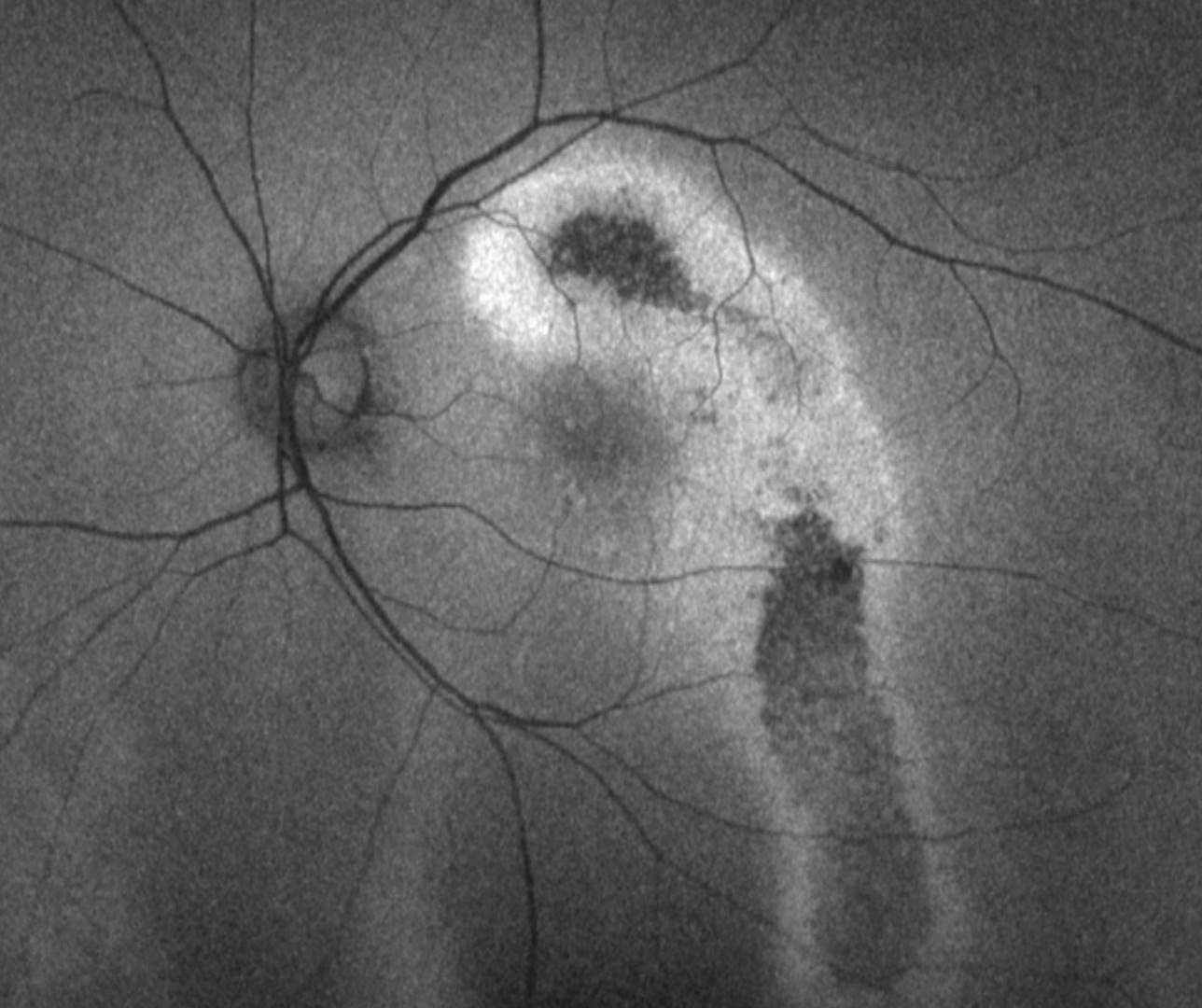
Fundus autofluorescence (FAF) imaging can show a multifocal or diffuse hypo-autofluorescence representing atrophy of the RPE. There may also be hyper-autofluorescence. The FAF pattern can descend inferiorly forming a gravitational tract that is characteristic of chronic CSCR.
Case Examples
-
Case 1: Chronic CSCR with gravitational tract
A 51-year-old Asian male with best-corrected visual acuity in the left eye of 6/9.5 (20/32-)
-
Case 2: Chronic CSCR with RPE atrophy
A 58-year old Asian male with best-corrected visual acuity of 6/7.5- (20/25-) in the right eye.
-
Case 3: CSCR complicated by CNV
A 48 year old Asian male with a history of long-standing CSCR in the left eye. His best corrected visual acuity is 6/7.5- (20/25-). A cortical cataract is noted inferiorly in the left eye.
Differential Diagnosis
References
Borooah, S, Sim, P.Y, Phatak, S, Moraes, G, Wu, C.Y, Cheung, CMG., Pal, B, Bujarborua, D. (2020), Pachychoroid spectrum disease. Acta Ophthalmol.
Cheung, CMG, Lee, WK, Koizumi, H. et al. Pachychoroid disease. Eye 33, 14–33 (2019).